Bariatric Center Spotlight: Fairfield County Bariatrics, Southern Connecticut
by Abe Fridman, DO, FACS, FASMBS
Dr Abe Fridman is a partner at Fairfield County Bariatrics and is the Director of Bariatric Surgery at Griffin Hospital in Derby, CT.
Funding: No funding was provided.
Disclosures: The author reports no conflicts of interest relevant to the content of this article.
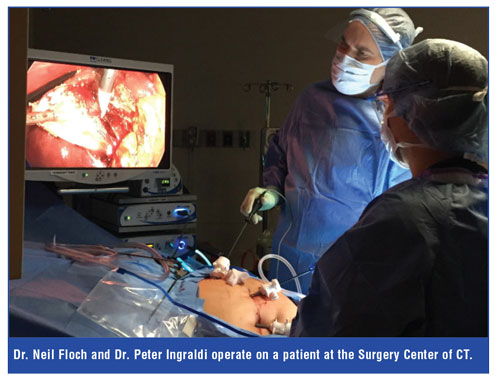 Welcome to Fairfield County Bariatrics
Welcome to Fairfield County Bariatrics
Fairfield County Bariatrics is a private bariatric and general surgery practice in southern Connecticut. Our practice offers an array of weight loss options (e.g., surgery, endoscopic treatments, and nonsurgical weight loss) to patients. Our patients come from Connecticut and surrounding states, including New York, Massachusetts, and Rhode Island. The practice began as a general surgery practice in 1994 with Dr. Craig Floch. We began performing bariatric surgery in 2002 and have been growing ever since. Our physicians are program directors at four different American College of Surgeons (ACS) and American Society for Metabolic and Bariatric Surgery (ASMBS) Metabolic and Bariatric Surgery Accreditation and Quality Improvement Program (MBSAQIP) accredited institutions across the state. We perform outpatient bariatric procedures and endoscopies at two separate ambulatory surgery centers. Our practice has three bariatric surgeons, two general surgeons, a physician assistant, a patient advocate team, and several dietitians and clinical psychologists with whom we partner in the communities we serve and at the hospitals in which surgeries are performed.
 Our Staff
Our Staff
Craig L. Floch, MD, FACS, was raised in Connecticut and started the practice in 1994. He has been a strong leader and is responsible for much of the growth of the practice across the state. He is the director of bariatric surgery at St. Vincent’s Medical Center in Bridgeport, Connecticut. Dr. Craig Floch has recently started seeing patients in the Danbury office for the Western Connecticut Health Network. He has performed thousands of bariatric procedures over the years, including laparoscopic Roux-en-Y gastric bypass (LRYGB), laparoscopic sleeve gastrectomy (LSG), and laparoscopic adjustable gastric banding (LAGB). Dr. Floch also performs robotic bariatric procedures.
Neil Floch, MD, FACS, joined his brother, Craig, in practice in 1998, and together they built the bariatric surgery service line of the practice, beginning in 2002. Dr. Floch is the director of bariatric surgery at the Western Connecticut Health Network, which includes Norwalk Hospital and Danbury Hospital. Dr. Neil Floch completed his fellowship in advanced laparoscopy at the Mayo Clinic Campus in Florida under Dr. Ron Hinder. He has performed thousands of bariatric surgeries and endoscopies, as well as revisional procedures.
Abraham Fridman, DO, FACS, FASMBS, joined the group in 2012 after completing his bariatric surgery fellowship at Cleveland Clinic Florida under Dr. Raul Rosenthal. He is the director of bariatric surgery at Griffin Hospital in Derby, Connecticut. He has performed hundreds of bariatric procedures since joining the practice. Dr. Fridman was the first physician in the state of Connecticut to perform placement of an Orbera Intragastric Balloon (Apollo Endosurgery, San Diego, California). He and Dr. Neil Floch perform these procedures for the practice.
Peter Ingraldi, MD, FACS, is a trauma and acute care surgeon. He is one of the few double-boarded surgeons in the state. Dr. Ingraldi is board certified in general surgery and critical care. He is an integral part of the practice, providing coverage of general surgery and trauma services in multiple facilities.
Marko Lujic, MD, joined the practice beginning in October of 2017. He is a general surgeon who completed his undergraduate studies, residency, and internship at Yale University. He is also a native of Connecticut, having grown up in the North Haven area, and looks forward to expanding the service area of the practice to the Milford area along with his partners.
Amanda Christie, PA-C, is a very important part of our practice. She provides care to many bariatric surgery patients, both preoperatively and postoperatively. She is truly passionate about the treatment of morbid obesity and is an asset to our practice and our patients. She is compassionate, supportive, and has a strong background in nutrition and primary care.

Our Bariatric Patient Navigation Team supports patients throughout the workup process up to the scheduling of surgery. This team is led by Julie Sjoblom and includes Sherah Rodriguez, Dawn Robinson, Anita Gilchrist, and our surgical scheduler, Vee Lusniak. The role of this team is to assist patients throughout the work-up process and help them understand the requirements of their specific insurance. We work with patients and providers to ensure medical clearance and testing is completed in a timely manner. This team is seasoned, has considerable experience and knowledge of the requirements for insurance providers in the state, and is available to assist our patients at all levels. This group also will work with patients on any insurance issues and will assist with any appeals if required.
Our practice partners with several dietitians and clinical psychologists in the area who have vast experience with morbid obesity and bariatric surgery. We meet with these clinicians on an annual basis and are available to discuss individual cases as well. We work hard to collaborate and ensure that we are up to date with the latest guidelines and recommendations. These providers are essential to the success of our patients by educating and preparing patients for bariatric surgery. We value their input and care and encourage all of our patients to see their dietician and mental health provider preoperatively and postoperatively.
We offer nutritional counseling and support at each hospital we partner with, including Danbury Hospital. Many patients see Tamara Swett at Norwalk Hospital, Karen Novack provides nutrition guidance at St. Vincent’s Medical Center, and Larissa Zepko-March and Kate Kelley offer services at at Griffin Hospital. In addition to these providers, we work with private practitioners, including Lynn Holmberg in Norwalk, Nancy Murphy in Fairfield, Kathy Kraus in Stamford, Lynda Mezansky in Stamford, and Jane Conway in Fairfield, among others.
For mental health services, some of the hospitals allow for outpatients to access their providers, where others direct patients to providers in the outpatient setting. In the Norwalk area, Lisa Mandelman cares for many of our patients. In the Stamford area, Janet Bertoldi provides care and treatment. In the Fairfield area, we have Dana Zuskin and Jane Conway. At Griffin Hospital, Kelly Miller is available for consultation. In the New Haven area, Dr. Mark Gaynor and Dr. Angelica Kaner consult our patients.
 A Unique Facility
A Unique Facility
Each bariatric program with which our practice is affiliated is fully accredited and has a bariatric coordinator who monitors the program and ensures compliance with all MBSAQIP standards and requirements. Barbara Vala is the bariatric coordinator at Norwalk Hospital, Mary Lou Viola is the bariatric coordinator at Danbury Hospital, Victoria DiNardo is the bariatric coordinator at St. Vincent’s Medical Center, and Kimberly Fisher is the bariatric coordinator at Griffin Hospital.
We have two primary offices at which we see most of our patients. Our flagship location is in Norwalk, Connecticut, and our secondary office is in Shelton, Connecticut. Each office is equipped with bariatric chairs and tables, including multiple scales that go up to 1,000 pounds. Each facility does annual sensitivity training, and our staff is fully capable of managing patients with various degrees of severity of morbid obesity.
Patient Demographics
We perform LRYGB, LSG, and LAGB. We also offer revisional and conversion procedures for patients who have not met their goals with a primary bariatric surgery. As a practice, we perform over 400 bariatric procedures on an annual basis. We take care of patients with all insurances across the region and offer affordable private-pay pricing packages for patients who do not have insurance coverage for bariatric services.
An Accredited Center
We have been designated as a Center of Excellence/Accredited program since 2002. We pride ourselves on our ability to meet and comply with the requirements set forth by the ASMBS/ACS/MBSAQIP. We have met and maintained the high standards required to keep these designations in good standing. We are proud to provide our patients great surgical care at multiple accredited centers across the state. Our patients know the significance of this designation at these facilities and the benefits of having their surgery at an accredited center.
Patient Adherence
The electronic medical record (EMR) system we have in place at our practice is NextGen (NextGen Healthcare, Horsham, Pennsylvania). This, in combination with unique internal tracking systems, allows us to monitor patient progress throughout the work-up process, as well as track adherence to postoperative follow-up care. We have also recently added a Patient Portal for patients to increase access to appointment scheduling and communication with the practice. We work hard to make sure patients follow the postoperative appointment schedule to stay on track and be successful. If a patient has not been seen in a while, we will continually reach out to him or her via telephone and mail to encourage adherence and proper care.
The biggest obstacle to caring for patients with morbid obesity in Connecticut is the issue of insurance coverage. Since we started performing bariatric surgery, we have kept track of patients who attend our seminars. Many attendees would qualify for the procedures but have an exclusion on their health insurance policy. Connecticut does not offer coverage for bariatric services on the health exchange plans. Unfortunately, these two factors greatly limit who is able to have surgery. In our state, only about 30 to 40 percent of patients with insurance have coverage for bariatric surgery. We advocate and fight for increased access to coverage for bariatric services and encourage patients to be outspoken as well.
 Patient Process
Patient Process
All of our patients attend a free informational seminar or view an online seminar prior to coming to the office for a consultation. These seminars are offered in different hospitals and other venues across the state. Our online seminar provides access for patients to learn about morbid obesity, bariatric surgery, and the various procedures available, all in the comfort of their own home. We collect insurance information and basic demographic information at the seminar, and then our team then calls each individual’s insurance plan to verify coverage and get details on benefit plans for the patients prior to scheduling an appointment. If a patient does not have coverage, our team will work with the patient and his or her employer to find a solution to any coverage issues that might prevent the patient from accessing proper treatment. All first consultation appointments are one-on-one visits with the surgeon. An individualized work-up is outlined and discussed. The full medical history of the patient is reviewed, and there is an opportunity for questions and concerns to be discussed with the physician directly. We guide patients through a full medical, nutritional, and psychological work-up in preparation for bariatric surgery. Our staff is easily accessible and is in touch with patients throughout the work-up. We are available to assist with referrals, surveillance of appointments, and clearance. Once the work-up is complete, we open a case and submit the patient’s file to the insurance company for approval. When approvals are received, our surgical coordinator contacts the patient and schedules an appointment for a preoperative visit with the surgeon, as well as a surgery date and the first two postoperative visits. The first postoperative visit is with the surgeon 7 to 10 days following the procedure, and the second postoperative visit is with our physician assistant approximately five weeks after the surgery. Preoperative visits take place approximately 2 to 3 weeks prior to surgery. At the preoperative visit, questions are answered, work-up and clearance is reviewed in detail, and consents are signed. We encourage all patients to attend support groups on a regular basis. These meetings are available at all facilities where we provide care. We take great pride in our surgeons being available to always answer the calls, nights, weekends, and all holidays. A member of our clinical team is available 24 hours a day, seven days a week, 365 days a year.
New Technologies
We perform the Orbera Intragastric Balloon (Apollo EndoSurgery, San Diego, California) and the Obalon Balloon System (Carlsbad, California). Dr. Fridman was the first surgeon to perform the procedure in the state. We offer our patients endoscopic revisions of LRYGB with the Overstitch device from Apollo (San Diego, California) to help patients who struggle after their primary procedure. Our practice offers medical weight loss options for patients who do not qualify for surgery or who might not be ready for surgery. We follow the patient regularly with nutritional counseling, weight loss medication, and regular visits, as needed.
We believe that bariatric surgery, like everything else, is always evolving. We offer our patients the latest options in the field. Nowadays, with more nonsurgical options, patients are looking for “less surgery” for the treatment of morbid obesity. As the interest and demand for more endoscopic procedures increases, there will be an increase in investigation and implementation. However, the long-term success of these procedures warrants further study.
An Interesting Case
Dr. Fridman had an interesting and difficult case in his first few months out of fellowship. The patient was a young woman who had undergone an LRYGB many years ago in South America. She presented with abdominal pain, nausea, and vomiting for several months. The patient had not seen a bariatric surgeon and had had numerous tests ordered by her primary care physician and gastroenterologist, of which all were negative. The patient then presented to an emergency room with the same symptoms. This time her computed tomography (CT) scan showed a questionable internal hernia and small bowel obstruction. There also appeared to be bowel ischemia. The patient was transferred to one of our facilities for a diagnostic laparoscopy. Intraoperative findings revealed an internal hernia through Petersen’s space with ischemic roux limb and part of the common channel. Dr. Fridman consulted with Dr. Neil Floch, given the extent of the ischemia. A decision was made to excise the whole roux limb and to reverse the gastric bypass. The operation went well and was entirely laparoscopic. The patient recovered with no complications and was discharged home. At the 18 month follow-up visit, she was keeping her weight off and was doing well.
Conclusion
When a patient makes the decision to see one of our surgeons, they become a part of our team, our family. Our practice began with two brothers, and our “family” continues to grow. We embrace each patient and their individuality, continually encouraging and supporting them before, during, and after surgery, so that they can achieve the success they so richly deserve. Our strong support system offers many options to our “family members” as they travel on their weight loss journey to regain their health and recapture their lives. Throughout their journey, our patients are never alone. Our surgeons, physicians, and staff are with them every step of the way, helping our patients create a life that is full of health, happiness, and adventure. We are grateful to share in the lives and success stories of so many family members.
Category: Bariatric Center Spotlight, Past Articles







