My Experience Performing the First Telesurgical Procedure in the World
by Jacques Himpens, MD, PhD
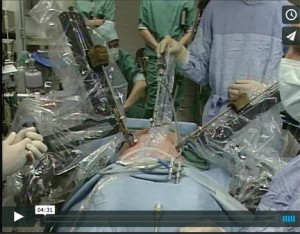
Watch the Video: Robotic Laparoscopic Cholecystectomy
 Jacques Himpens, MD, PhD, is an Associate Professor of Surgery at the European School of Laparoscopic Surgery and Chief of Bariatric Surgery at the CHIREC Hospital, Brussels, Belgium, and St. Blasius General Hospital, Dendermonde, Belgium. In 1977, he graduated cum laude from the Catholic University of Leuven, Leuven, Belgium. In 1992, after six years in private practice in Belgium, Dr. Himpens joined the Université Libre de Bruxelles. He became an attending surgeon at the St. Pierre University Hospital Brussels. He assisted Dr. Guy-Bernard Cadière with the world’s first laparoscopic adjustable band gastroplasty in October 1992. On March 3, 1997, Dr. Himpens performed the world’s first “robotic” laparoscopic cholecystectomy using an early robot system prototype. He performed the first laparoscopic gastric bypass in Belgium in 1999, and the first laparoscopic biliopancreatic diversion with duodenal switch in 2001. He has performed over 15,000 laparoscopic obesity procedures, many of them revisional. He has had over 150 articles published in peer-reviewed medical journals, authored a substantial number of chapters in surgical books, and co-edited four books on bariatric surgery. He is co-editor for Obesity Surgery and is a member of the editorial board of Surgery for Obesity and Related Diseases.
Jacques Himpens, MD, PhD, is an Associate Professor of Surgery at the European School of Laparoscopic Surgery and Chief of Bariatric Surgery at the CHIREC Hospital, Brussels, Belgium, and St. Blasius General Hospital, Dendermonde, Belgium. In 1977, he graduated cum laude from the Catholic University of Leuven, Leuven, Belgium. In 1992, after six years in private practice in Belgium, Dr. Himpens joined the Université Libre de Bruxelles. He became an attending surgeon at the St. Pierre University Hospital Brussels. He assisted Dr. Guy-Bernard Cadière with the world’s first laparoscopic adjustable band gastroplasty in October 1992. On March 3, 1997, Dr. Himpens performed the world’s first “robotic” laparoscopic cholecystectomy using an early robot system prototype. He performed the first laparoscopic gastric bypass in Belgium in 1999, and the first laparoscopic biliopancreatic diversion with duodenal switch in 2001. He has performed over 15,000 laparoscopic obesity procedures, many of them revisional. He has had over 150 articles published in peer-reviewed medical journals, authored a substantial number of chapters in surgical books, and co-edited four books on bariatric surgery. He is co-editor for Obesity Surgery and is a member of the editorial board of Surgery for Obesity and Related Diseases.
The History of Bariatric Surgery
This column is dedicated to telling the stories of leaders who have helped shape the field of bariatric surgery through their discoveries, teaching, and stewardship.
Column Editor: George L. Blackburn, MD, PhD, FACS
S. Daniel Abraham Professor of Nutrition; Associate Director, Division of Nutrition Harvard Medical School; Director, Center for the Study of Nutrition Medicine, Department of Surgery, Beth Israel Deaconess Medical Center, Boston, Massachusetts
Column Editor: Daniel B. Jones, MD, MS, FASMBS
Professor of Surgery, Harvard Medical School, Vice Chair, Beth Israel Deaconess Medical Center, Boston, Massachusetts
A Message from the Column Editors
Dear Readers of Bariatric Times:
Bariatric surgery has many leaders who have shaped the field by their discoveries, teaching, and stewardship. In this column, we invite leaders to tell us about their most significant accomplishment(s). Here, we will hear from leaders about their visions, hurdles, collaborations, and, ultimately, what impact their accomplishments have had on the field of bariatric surgery. We will also learn how they set goals and have turned ideas into reality, as well as what was anticipated and what was not expected throughout their journeys.
We are very excited about this project and hope it will help to inspire the next generation of leaders as they evaluate new devices and technology and consider novel procedures and treatments in an era of cost containment. We hope you enjoy these stories.
Sincerely,
Drs. George L. Blackburn and Daniel B. Jones
One of the major limitations of conventional laparoscopic surgery is the reduction of the number of degrees of freedom to move instruments inside the abdominal (or chest) cavity. Degrees of freedom are limited by the fixed entry points through which the long, non-articulated tools are introduced. This situation creates a mobility pattern that resembles that of an open procedure performed by a surgeon’s hand that is fixed in all its joints. Articulated laparoscopic tools while designable cannot be manipulated under normal conditions because the different articulations demand separate handles that must be operated simultaneously, a situation that cannot be managed by the human brain and by one pair of hands. The interposition of a computer-driven interface, however, may allow for such complex manipulation patterns.
In 1995, a physician who had understood the commercial value of the emerging robotic technology, Frederic H. Moll, MD, acquired the license to the telepresence robotic surgical system developed by the NASA-SRI teams, and started a company called Intuitive Surgical Inc.® (Intuitive Surgical Inc., 2005; Satava, 2003). Intuitive Surgical Inc. used the telepresence robotic technology pioneered by the NASA-SRI team to develop a master-slave telepresence robotic surgical system.[1]
Thanks to the computer interface, complex motions of an individual’s (i.e., a surgeon) hands and fingers (the master) are translated to an effector system that accurately and three-dimensionally transmits the impulses needed for the activation of articulated tools (the slave). Moreover, the computer allows for downscaling of the master’s motions, which can result in miniature motions of the slave-tools mimicking the master’s manipulations performed with greater amplitude. Downscaling may be useful in carrying out microsutures as in vascular anastomosis. Conversely, small oscillations of the master’s hands (as caused by physiologic trembling) may be eliminated by the computer interface.
Computer-guided telepresence had captured my interest since the Society for Minimally Invasive Therapy (SMIT) meeting held in Dublin, Ireland, in November 1992. Hence, when I was approached by Dr. Moll the following year concerning the recent developments in telepresence surgery, I was immediately interested. I had met Dr. Moll through my contacts with the Origin company (at the time I was substantially involved in the totally extraperitoneal inguinal hernioplasty or TEPP procedure and the Origin company were the manufacturers of the balloons we used for creation of the extraperitoneal space). Since Dr. Moll knew me personally from numerous workshops organized by Origin, he introduced me to the SRI technology that he was interested in acquiring. I obviously shared his enthusiasm and encouraged him to purchase the revolutionary robot system. In 1995, Dr. Fred Moll eventually acquired the full license to the telepresence NASA-SRI system. He gathered a crew of keen and enthusiastic medical engineers and started working on the development of a system that would be usable in human surgery. Shortly thereafter I met with the entire Intuitive team (a mere 5 people, all engineers) and we discussed a strategy to eventually use the robot technology in humans. The name of the prototype robot was Mona (Intuitive, Mountain View, California) in analogy with the Mona Lisa, Da Vinci’s masterpiece. Da Vinci was not only a talented renaissance painter, but also a keen inventor, and he is considered by some the father of the robot. (Quite logically, the name of the telepresence system was later changed to “Da Vinci”)
In 1997, the performances of the Intuitive master-slave computerized system had reached a level that rendered its use feasible and apparently safe in a human model. Dr. Moll and I decided to go for it and thought it would be wise to focus on rather simple procedures.
When I first introduced to the local ethical committee the demand to perform “robotic surgery” in my clinical practice in Dendermonde, Belgium (a private care facility), the members of the committee initially assumed I had gone insane (which, in hindsight, may very well have been the case). However, after reviewing the outcomes of substantial animal testing with the telepresence system performed in the United States, the institutional review board of the St. Blasius hospital at Dendermonde, Belgium released the authorization for performing a number of computer-guided, simple surgical procedures, including laparoscopic cholecystectomy, lysis of adhesions, and the performance of an arteriovenous fistula for dialysis access, in five consenting patients who were duly informed on the experimental aspect of the endeavour.
On March 3, 1997, I successfully performed the first “robotic” laparoscopic cholecystectomy on a 52-year old female patient who suffered from symptomatic cholecystolithiasis.[2] I performed the surgery at some 10 yards away from the patient, while sitting at the master’s console. In the meantime, a second surgeon, Dr. Guido Leman, was standing at the patient’s side to hold the camera and to provide assistance in case of technical mishaps. The effector system consisted of two articulated robot arms to which the sterile tools had been snapped. At the time, the tools consisted of a grasper and a coagulating hook mounted at the end of articulated “endo-wrist” mechanisms that had been introduced inside the patient’s abdomen through conventional trocar cannula’s placed by the first author at the beginning of the procedure. The procedure was performed under guidance of a 3D optical system that required the use of adjusting goggles to obtain an in-depth view of the surgical field.
Minor problems were encountered, such as imperfect insolation of the hook that had to be covered by the tip of a glove that was tied to the endo-wrist system. The grasper tip (the grasper was actually a needle holder) was found to be too sharp to allow common use. However, the procedure was concluded successfully in 65 minutes, and the patient made an uneventful recovery.
The same day, an additional laparoscopic cholecystectomy and a lysis of adhesions were performed without incidents. Two cases of arteriovenous fistula were also successfully performed the next day.
The experiment was judged satisfactory and company clearance was given for the continuation of the project.
I submitted the report on the world premiere to several journals including the New England Journal of Medicine and the Lancet, but the paper was both times refused because it was judged “inappropriate” or “very unlikely to have actually happened.” Eventually, the report was published in the journal Surgical Endoscopy as a letter to the editor.[2] Conversely, the “robot world’s first” made it to the evening news on the VRT, the national Flemish television channel, which gave the whole event at least some echo in the lay press.
The engineers from Intuitive carefully addressed the insolation issue and tried to develop effector tool tips that would better accommodate their intended use. As a next step, a more complex procedure, including suturing was planned. I introduced my friend and partner at the St. Pierre University hospital, Dr Guy-Bernard Cadière, to the project and got him involved with the research of the Intuitive Company. Guy-Bernard is an enthusiastic surgeon and scientist who had acquired international fame in Nissen fundoplication, and in other advanced laparoscopic surgeries. He had performed the first laparoscopic adjustable gastric banding procedure in October 1992,[3] and I had had the chance to scrub on the case.
In May 1998, Dr. Cadière performed a telepresence Nissen fundoplication at Broussais hospital in Paris, France. The system used then had significantly been improved as it comprised an upgraded console allowing binocular 3D direct vision and the use of a third robotic arm for manipulation of the optical system. The incorporation of a third robotic arm rendered the presence of a surgeon at the patient’s side obsolete.
After successful completion of the advanced procedure, clearance was given by the St. Pierre University hospital for further use in selected patients planned to undergo a variety of more complex operations, including an adjustable band gastroplasty, which constituted the first “robotic” bariatric procedure.[4]
A significant number of procedures were subsequently performed by Dr. Cadière and myself, and we gathered our experience and impressions in an article published in World Journal of Surgery.[5]
Further advancements from then on included the inclusion of a fourth robot arm, further improvement of the 3D optical system into high definition, and the implementation of stapling and ultrasonic-scissors technology in the effector system. The robot arms themselves no longer needed to be separately fixated on the operating table side bars as they were mounted on a “side cart” that could easily be advanced over the patient.
Needless to say, after our initial “try-outs,” robotic surgery made a gigantic leap forward. Today, a simple Medline search of the term robotic surgery reveals some 8,643 citations (ironically, you will not find the report on the very first robotic laparoscopic cholecystectomy in that list.)
Nevertheless, unlike urologists who massively adopted the technique of “robot prostatectomy,” most gastro-intestinal surgeons are still reluctant to use the Da Vinci system in everyday practice because no clear evidence of added benefit of using robot technology has yet been shown for most surgical procedures. The bulk of the system, practical concerns around the “docking” procedure, and, of course, financial issues remain deterring factors. The future will tell us if further advances, such as the implementation of the “one port” technique will outweigh the downsides.
References
1. The Official Medical Robotics News Center for AVRA Surgical Robotics Inc. http://allaboutroboticsurgery.com/
surgicalrobots.html. Accessed March 17, 2016.
2. Himpens J, Leman G, Cadiere GB. Telesurgical laparoscopic cholecystectomy. Surg Endosc. 1998;12(8):1091.
3. Cadière GB, Bruyns J, Himpens J, Favretti F. Laparoscopic gastroplasty for morbid obesity. Br J Surg. 1994;81(10):1524.
4. Cadière GB, Himpens J, Vertruyen M, Favretti F. The world’s first obesity surgery performed by a surgeon at a distance. Obes Surg. 1999;9(2):206–209.
5. Cadière GB, Himpens J, Germay O, et al. Feasibility of robotic laparoscopic surgery: 146 cases. World J Surg. 2001;25(11):1467–1477.
Category: History of Bariatric Surgery, Past Articles




