Among Patients Diagnosed with Obesity, Higher Disease Burden was Associated with More Referrals to Adult Weight Management Programs (AWMPs)

by Amanda Velazquez, MD, DABOM, and Jennifer J. Kim, MA
Dr. Velazquez is Director of Obesity Medicine, Comprehensive Weight Loss Center, Cedars Sinai Medical Center in Los Angeles, California. Ms. Kim is Senior Data Consultant, Southern California Kaiser Permanente in Pasadena, California.
Funding: No funding was provided for this article.
Disclosures: Dr. Velazquez is on the advisory board for Intellihealth.
Bariatric Times. 2022;19(9):10–11.
Abstract
Objective: The goal was to evaluate the relationship between disease burden among patients with obesity and the referral rates by primary care providers (PCPs) to adult weight management programs (AWMPs) and assess the relationship between disease burden and attendance rates to AWMPs of those patients referred.
Design: The study was a retrospective review of Southern California Kaiser Permanente West Los Angeles Hospital (KP WLA) electronic medical records (EMRs).
Setting: Los Angeles, California.
Participants: There were 26,767 adult patients (≥18 years of age) with obesity (body mass index [BMI]≥35kg/m2) between January 1, 2015, and December 31, 2018. Participants were categorized into three groups, ranging from higher to lower disease burden: severe obesity (BMI≥40kg/m2), obesity (35kg/m2≤BMI<40kg/m2) plus two or more comorbidities, and obesity (35kg/m2≤BMI<40kg/m2) plus one comorbidity.
Measurements: BMI, disease burden (i.e., comorbidities), rates of diagnosis, referrals, and attendance.
Results: Of the 11,225 patients with a BMI of 40kg/m2 or greater, 74.7 percent (n=8,387) were diagnosed with obesity; 68.8 percent (n=5,774) were referred to AWMPs, and of those patients, 20.0 percent (n=1,157) attended AWMPs. Of the 13,759 patients with a BMI between 35kg/m2 and 40kg/m2 plus two comorbidities, 60.9 percent (n=8,383) were diagnosed with obesity; 65.2 percent (n=5,466) were referred to AWMPs, and of those patients, 12.0 percent (n=658) attended AWMPs. Of the 1,783 patients with a BMI between 35kg/m2 and 40kg/m2 plus one comorbidity, 56.3 percent (n=1,004) were diagnosed with obesity; 37.6 percent (n=378) were referred to AWMPs, and of those patients, 3.70 percent (n=14) attended AWMPs.
Conclusion: Among patients diagnosed with obesity, those with higher disease burden were more often referred to AWMPs and similarly achieved higher attendance rates to these programs. Greater research is warranted to understand and address barriers to improving referral rates to AWMPs, as well as increasing attendance to these programs.
Keywords: Obesity treatment, weight management, primary care, bariatric surgery, comorbidities, weight management, referral patterns
Obesity is a chronic, relapsing disease that affects 42 percent of adults in the United States (US).1 As physicians, there is the utmost urgency to recognize and treat obesity. About 55 percent of physician office visits in the US take place in primary care offices,2 making it the ideal setting to initiate a conversation about weight, diagnose obesity, and discuss various treatment modalities. The first step in addressing obesity is identifying the disease. In doing this, documenting an obesity diagnosis code in the electronic medical record (EMR) is crucial.
Research demonstrates that entering an obesity diagnosis code is a strong predictor for formulating an obesity plan,3 including placing a referral to adult weight management programs (AWMPs). It has also been found that among patients with obesity (body mass index [BMI]≥35kg/m2), those with higher disease burden are more likely to have an obesity diagnosis code entered.3–5 However, among patients with an obesity diagnosis entered by a primary care provider (PCP), it is unknown if disease burden is associated with referral and attendance rates to AWMPs. Of the patients diagnosed with obesity, we hypothesized that those with a higher disease burden would be more likely to receive a referral from a PCP and attend AWMPs.
Methods
Souther California Kaiser Permanente West Los Angeles Hospital (KP WLA), located in Los Angeles, California, is comprised of an ethnically diverse population of 230,000 patients. Between January 1, 2015 and December 31, 2018, we analyzed data from 26,767 KP WLA patients to conduct a retrospective review of all adult patients (≥18 years of age) who met criteria for our classification of disease burden. Participants were categorized into three groups, ranging from higher to lower disease burden: patients with severe obesity (BMI≥40kg/m2); patients with obesity (35kg/m2≤BMI<40kg/m2) and two or more established, weight-related comorbidities; and patients with obesity (35kg/m2≤BMI<40kg/m2) and one established, weight-related comorbidity. Weight-related comorbidities include Type 2 diabetes, hypertension, and obstructive sleep apnea (OSA), among others.6
First, we assessed which patients received a diagnosis code of obesity entered by a PCP during the time period of interest. A diagnosis code for obesity is defined by the International Statistical Classification of Diseases (ICD) codes entered during a medical encounter with a PCP. When a patient had multiple BMIs due to multiple primary care visits in the study period, the most recent BMI was used. Only Medicare patients, (making up less than about 15% of our patient population) received an EMR prompt to enter a diagnosis of severe obesity (BMI≥40kg/m2) or obesity (35kg/m2≤BMI<40kg/m2) with one or more comorbidities. A prompt is satisfied once a provider enters the diagnosis code during a patient encounter. This prompt will not reissue until the start of the new calendar year. To evaluate the degree of disease burden with weight-related comorbidities, the problem list was reviewed for any of the following ICD-10 codes: Z71.3,E66.9, Z68.54, Z68.30, Z68.31, Z68.32, Z68.33, Z68.34, Z68.35, Z68.36, Z68.37, Z68.38, Z68.39, Z13.21, E66.01, E66.09, E66.1, E66.2, E66.8, Z68.41, Z68.42, Z68.43, Z68.44, Z68.45, Z98.84, Z90.3.
Among patients with an obesity diagnosis code entered, we assessed the relationship of disease burden to the rate of referral to AWMPs by PCPs. AWMPs were defined as one of five, virtual or in-person, weight management support programs at KP WLA. Each program is unique, but all have a common theme of weight-loss counseling (Table 1). Patients in the three groups of varying disease burden all met criteria to participate in any of the AWMPs listed in Table 1.
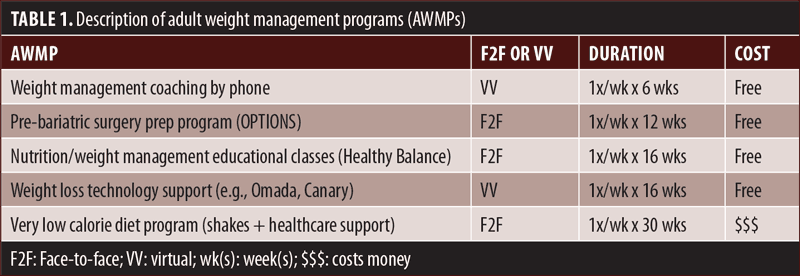
When discussing attendance of the three patient groups of varying disease burden, we refer to attendance in its entirety (all sessions). Attendance was not evaluated individually but as a sum. There were five different types of programs (Table 1) included in our analysis, one of which was the preoperative program for bariatric surgery; this 12-week class series and/or a consult with a bariatric surgeon are required to be completed by any patient interested in pursuing bariatric surgery. Lastly, referral to AWMPs might not be from the same encounter that an obesity diagnosis code was entered.
Results
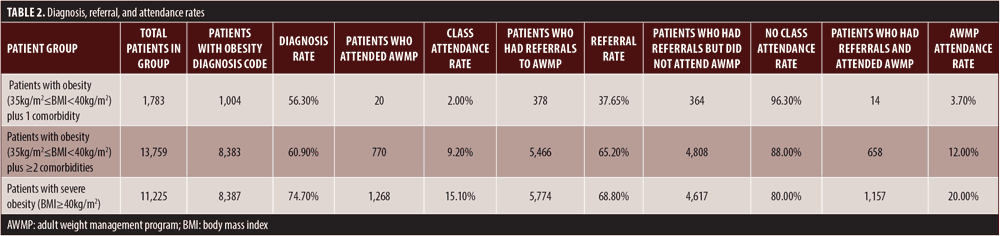
See Table 2 for details of our findings, listed in three categorized groups, from higher to lower disease burden.
Patients with severe obesity. Among the 11,225 patients with a BMI of 40kg/m2 or greater, 74.7 percent (n=8,387) were diagnosed with obesity. Of those diagnosed, 68.8 percent (n=5,774) were referred to AWMPs, and of those patients, 20.0 percent (n=1,157) attended an AWMP.
Patients with obesity and two or more comorbidities. Among 13,759 patients with a BMI between 35kg/m2 and 40kg/m2 plus two or more comorbidities, 60.9 percent (n=8,383) were diagnosed with obesity. Of those diagnosed, 65.2 percent (n=5,466) were referred to AWMPs and of those patients, and 12.0 percent (n=658) of them attended an AWMP.
Patients with obesity and one comorbidity. Of 1,783 patients with a BMI between 35kg/m2 and 40kg/m2 plus one comorbidity, 56.3 percent (n=1,004) had a diagnosis of obesity. Of those diagnosed, 37.6 percent (n=378) were referred to an AWMP, and of those patients, 3.70 percent (n=14) attended an AWMP.
Discussion
Diagnosis rates. Our data re-establishes previous findings3–5 that patients with obesity and higher disease burden have a high rate of receiving an obesity diagnosis code entered by PCPs. Low confidence among PCPs in their skills to discuss weight and/or knowledge of available treatments for obesity could explain the continued trend established in the literature. Importantly, before and during the study, PCPs at KP WLA had yet to receive any formal training on how to discuss weight and treatment options with patients in a nonbiased, approachable manner.
Referral rates. Our primary aim was to assess the association of disease burden of patients with obesity and referral rate to AWMPs. We found that among patients diagnosed with obesity, higher disease burden (BMI≥40kg/m2 and 35kg/m2≤BMI<40kg/m2 plus ≥2 comorbidities) was associated with more referrals to AWMPs by a rate of nearly double (68.8% and 65.2% vs. 37.65%) when compared to those with lower disease burden (35kg/m2≤BMI<40kg/m2 plus 1 comorbidity). We speculate that this could be due to a degree of weight bias, in which PCPs do not think patients with lower disease burden merit assistance through AWMPs because they should have the willpower to make changes on their own. However, when patients present with higher disease burden, PCPs may see fit that assistance is needed.
Attendance rates. Our secondary aim was to evaluate the association of disease burden among these patients referred to AWMPs with attendance rates of these programs. We found that those with higher disease burden were more likely to attend AWMPs. This could be for a myriad of reasons. Patients with higher disease burden may be more likely to be in an active state of readiness for behavior change, PCPs may be expressing low confidence in the effectiveness of AWMPs, and AWMPs may not be marketed adequately on a system level and/or have the content delivered in a way to gain patient buy-in when referred by their PCP.
Limitations. As a retrospective cohort analysis, this study is not without limitations. Referral to AWMPs was not from the same encounter as the original obesity diagnosis code entered by the PCP, which limits our interpretation of the data. In addition, attendance to AWMPs was evaluated not individually, but as one sum, making it difficult to know if one program was better attended than others.
Conclusion
In summary, our preliminary results show the referral rates of patients diagnosed with obesity with a BMI of 40kg/m2 or greater and those with a BMI between 35kg/m2 and 40kg/m2 with two or more comorbidities, compared to those with a BMI between 35kg/m2 and 40kg/m2 with one comorbidity, were nearly double (68.8% and 65.2% vs. 37.65%). Of those individuals referred to AWMPs, the patients with higher disease burden had the highest attendance rate. This data suggests that there is a missed opportunity to refer patients diagnosed with obesity and lower disease burden to AWMPs. These patients merit treatment options for their weight to improve overall health. Further research is warranted to better understand why this population is less likely to be referred by PCPs and strategize ways to improve attendance rates of patients with obesity to AWMPs.
Takeaway for Providers
- Consistent with prior data, patients with lower disease burden (35kg/m2≤ BMI<40kg/m2 plus 1 comorbidity) compared to those with higher disease burden (BMI≥40kg/m2 and 35kg/m2≤BMI<40kg/m2 plus ≥2 comorbidities) continue to be underdiagnosed during medical encounters with PCPs.
- Preliminary data demonstrated that among patients diagnosed with obesity, higher disease burden was associated with more referrals to AWMPs. This data suggests that there are missed opportunities to refer patients with obesity and lower disease burden to AWMPs accordingly.
- Of those individuals referred to AWMPs, attendance rates to these programs was uniformly low, and patients with higher disease burden had the highest attendance rate to AWMPs.
- There are limitations to this preliminary analysis, but concerted efforts are needed to better understand and address the barriers to referring patients diagnosed with obesity to AWMPs and improve their attendance rates to AWMPs.
References
- Hales CM, Carroll MD, Fryar CD, et al. Prevalence of obesity and severe obesity among adults: United States, 2017–2018. NCHS Data Brief, no. 260. National Center for Health Statistics; 2020. https://www.cdc.gov/nchs/products/databriefs/db360.htm. Accessed 4 Apr 2022.
- Rui, P, Okeyode T. National ambulatory medical care survey: 2016 national summary tables.https://www.cdc.gov/nchs/data/ahcd/namcs_summary/2016_namcs_web_tables.pdf. Accessed Jan 9 2022.
- Bardia A, Holtan SG, Slezak JM, Thompson WG. Diagnosis of obesity by primary care physicians and impact on obesity management. Mayo Clin Proc. 2007;82(8):927–932.
- Muo IM, Sacajiu G, Kunins H, Deluca J. Effect of the availability of weight and height data on the frequency of primary care physicians’ documented BMI, diagnoses and management of overweight and obesity. Qual Prim Care. 2013;21(4):221–228.
- McLaughlin JC, Hamilton K, Kipping R. Epidemiology of adult overweight recording and management by UK GPs: a systematic review. Br J Gen Pract. 2017;67(663):e676–e683.
- Centers for Disease Control and Prevention. Health effects of overweight and obesity. https://www.cdc.gov/healthyweight/effects/index.html. Accessed 15 Aug 2022.
Category: Brief Report, Past Articles




