How Do Postoperative Bariatric Patients Stay on Task with Nutrition Goals and Physical Activity to Prevent Weight Regain?

by Anthony L. Heard, EdD, RRT
Dr. Heard is a Registered Respiratory Therapist at Memorial Health University Medical Center in Savannah, Georgia.
Funding: No funding was provided for this article.
Disclosures: The author has no conflicts of interest relevant to the contents of this article.
Bariatric Times. 2023;20(7–12):16–21.
Abstract
Objective: The purpose of this research study was to explore how postoperative bariatric patients adhered to nutrition goals and physical activity to prevent weight regain. Obesity is a preventable condition that has become a worldwide epidemic. Bariatric surgery is the most effective tool for treating obesity when combined with diet and exercise.
Design: This qualitative study used thematic analysis and iterative comparison to identify the themes of motivation for surgery, support systems, eating habits, level of physical activity, mental health, physical health, health choices, and self-image to evaluate the challenges and successes of long-term weight loss after bariatric surgery.
Setting: The researcher used email correspondence to send the questionnaires to the participants and videoconferencing technology to conduct the interviews.
Participants: The participants included nine healthcare workers. Five participants were Black/African American, and four were White. One participant was male and eight were female.
Measurements: The researcher used QDA Miner Lite to compile and analyze the collected data to evaluate the challenges and successes of long-term weight loss after bariatric surgery.
Results: The data revealed that the participants who made unhealthy food choices and did not engage in physical activity gained 14 to 67 pounds. Those who made healthy choices and engaged in physical activity maintained their weight loss and did not experience weight regain.
Conclusion: Bariatric patients must understand that weight loss should be perceived as a life-long journey instead of a short-term method to achieve lasting results motivated by intrinsic and extrinsic factors.
Keywords: Bariatric patients, obesity, postoperative, weight regain
Bariatric surgery procedures have increased significantly because of the worldwide obesity epidemic. The American Society for Metabolic and Bariatric Surgery (ASMBS) estimated that physicians performed 158,000 bariatric procedures in 2011. There were 256,000 procedures performed in 2019, an increase of 98,000 surgeries in eight years.1 According to the World Health Organization (WHO), obesity has tripled since 1975, with almost two billion people with overweight and 650 million with obesity.2
In 2018, more than two-thirds of the American population identified as overweight, with a body mass index (BMI) of 25kg/m2 or higher, and one-third had obesity, with a BMI of 30 kg/m2 or higher.3 Bariatric procedures have significantly improved conditions such as diabetes, heart disease, hypertension, hyperlipidemia, obstructive sleep apnea (OSA), cancers, and fractures and reduced mortality outcomes among patients, compared to those who do not undergo surgery.4 Bariatric surgery is a more effective tool for controlling obesity than medication, diets, or exercise alone.4 Weight regain after bariatric surgery is a multifaceted issue influenced by surgery type, biology, behavior, environment, social network, socioeconomic, demographics, and more.5 Predicting which patients will successfully lose and maintain their weight is impossible. However, healthy eating habits and active lifestyles prevented weight regain after surgery, which was the perceived goal of the participants in this investigation. The purpose of this qualitative study was to evaluate how postoperative bariatric patients adhered to nutrition goals and physical activity to prevent weight regain.
Methods
The research methodology for this study used bariatric questionnaires and interviews to explore the challenges of maintaining long-term weight loss and preventing weight gain after bariatric surgery. This qualitative research approach used subjective methods and a small sample population to contextualize and interpret the data gathered for analysis. Aside from exploring the complexities of eating healthily and engaging in physical activity, the study brought awareness to psychosocial issues associated with obesity. The investigator used thematic analysis and iterative comparison to assess the participants’ experiences and behaviors with weight regain after bariatric surgery. This process allowed the researcher to make inferences about the group for publication and make suggestions for future investigations.6
Procedure. Aside from the initial self-reporting on the bariatric intake questionnaires, the researcher conducted interviews of all patients to ensure consistent data collection. The individual interviews were conducted online using Zoom (Zoom Video Communications, San Jose, CA, USA) videoconferencing technology. The software recorded the conversation and transcribed the dialogue into written text for further analysis. The interview questions and questionnaire were developed through a preliminary intake session with the researcher, a bariatric candidate who did not participate in the study, and another individual who had no personal interest in the study. The questions were beta tested, reviewed for biases, and did not influence the study results. The investigator used thematic analysis and iterative comparison to assess the participants’ statements without using a mixed-method study design. The semi-structured interview style allowed the researcher to go off script and ask probing questions about various topics to obtain in-depth information. Lastly, the researcher analyzed the interview data and sorted it into categories, giving rise to themes identified using the QDA Miner Lite software.
Sample. The study consisted of nine participants, five of whom were Black/African American and four of whom were White. One participant was male and eight were female. Eight participants had a sleeve gastrectomy procedure, and one had gastric bypass surgery. The recruiting process was conducted using convenience sampling after conversing with candidates who had bariatric surgery at the same place of employment as the researcher. The candidates had to be one-year post-bariatric surgery and at least 18 years of age to participate in the study. The only exclusion criterion for the research study was candidates less than one-year post-bariatric surgery because they were still healing and adjusting to food and liquid intake recommendations.
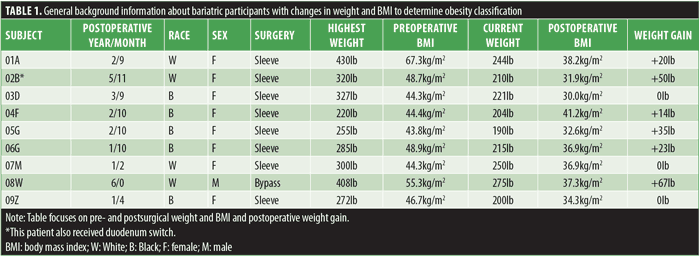
Research study. The participants in the study were healthcare professionals, and their BMIs were calculated using the weights and heights provided on the questionnaire. According to the Centers for Disease Control (CDC), a normal BMI ranges from 18.5 to 24.9 kg/m2. A BMI ranging from 25 to 29.9 kg/m2 indicates overweight, and a BMI of 30 kg/m2 or greater indicates obesity.7 The participants’ presurgical BMI ranged from 43.8 to 67.3kg/m2, showing that all the participants were classified as having morbid obesity (Table 1). Although the participants lost various amounts of weight, they were still classified as having obesity postsurgery, with BMI ranging from 30 to 41.2kg/m2. The classification of obesity reinforced the idea that preventing weight regain is essential to maintaining healthy weight postoperatively. Six participants gained 14 to 67 pounds after their bariatric procedure. The second participant underwent a gastric sleeve in October 2016. They gained 50 pounds after the initial procedure and decided to undergo a duodenum switch in April 2022. The duodenum switch combines the gastric sleeve with intestinal bypass to promote weight loss. That participant was accepted into the study because they received their initial procedure more than one year ago.
The interview questions were divided into primary themes: motivation for having bariatric surgery, support systems, eating habits, physical activity levels, mental and physical health, overall health choices, and self-image. The researcher asked questions about each theme to encourage a thorough conversation about participants’ relationships with food and physical activity.
Data analysis. The data analysis process evaluated the challenges and successes of weight loss after bariatric surgery using data collected from the questionnaire and individual interviews. The researcher used thematic and iterative comparisons to identify trends and compare findings by systematically analyzing aspects of the participants’ bariatric journeys to draw conclusions about the group for publication. The interviews were recorded, transcribed into written text, and uploaded to QDA Miner Lite for further analysis. Complex data was divided into usable codes that were easier to manage. The codes were grouped into overarching themes and divided into smaller categories to identify behavioral and emotional patterns. The researcher organized the themes and concepts into meaningful constructs.
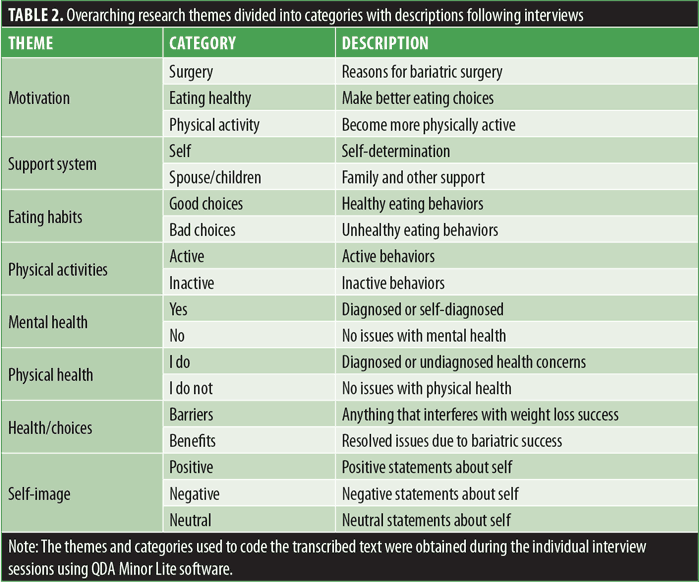
Descriptive analysis. QDA Miner Lite was used to sort, code, organize, and categorize all qualitative data. The interview data was divided into themes and categories to eliminate confusion when processing and analyzing information. The dominant themes identified from the interview questions were motivations for surgery, support system, eating habits, level of physical activity, mental and physical health, health choices, and self-image (Table 2). The data was funneled in themes and categories to understand the information better. Each category description explained the researcher’s thought process for coding the participants’ behaviors, feelings, attitudes, and patterns into meaningful assumptions.
Results
Through content analysis, the researcher quantified and analyzed the meaning of keywords and concepts without the presence of an inherent hypothesis. Central themes were explained, and the data was analyzed extensively. The quoted phrases are the exact words of the participants. The dialogue felt uninhibited and flowed effortlessly, revealing sensitive issues that contributed to obesity, including bullying, feelings of loneliness, verbal abuse, self-control issues, sexuality, using food as a coping mechanism, and sedentary lifestyles.
Motivation. Motivation is the self-regulation of human behavior to accomplish tasks or goals that are meaningful and continuous based on intrinsic and extrinsic factors.8 The motivation theme was divided into three categories: motivation for surgery, eating healthy, and physical activities. A review of that data showed that 89 percent of the participants had bariatric surgery for health reasons due to years of failed dieting, pain, discomfort, sleep apnea, shortness of breath on exertion, and other medical conditions. While improving overall health was an excellent motivator for bariatric surgery, six participants experienced weight gain postoperatively.
The participants were asked if circumstances or situations made them want to adhere more with healthy food choices and physical activities. The fifth participant said gaining weight after not fully adhering to dietary recommendations motivated them to get back on track. The third participant stated that upcoming outings, events, and trips motivated them to “kick it up a little bit” and increase adherence beyond expectations. The TV show My 600lb Life was a powerful motivator for the seventh participant. That participant compared their eating behaviors and mental state to individuals on the show and prayed they never ended up in like circumstances. Watching people binge eat, overindulge, fail to engage in physical activity, and make excuses for nonadherence motivated the seventh participant to stay on task with dieting and exercise. The second participant said the pain from overeating and the sick feeling from eating unhealthy foods reminded them they had overindulged. Overall, the participants planned to continue their journey despite challenges and setbacks that caused them to get off track.
Support system. A support system is a network of people who help bariatric patients overcome social, physical, and psychological obstacles throughout their weight loss journey while adjusting to their new lifestyles after surgery, especially during difficult times.9 The participants’ support systems were divided into self-support and family support systems. Self-support requires no explanation, while family support consists of spouses, children, and a cousin. All of the participants stated they felt their spouses and children supported them. However, they also felt solely responsible for their decisions to eat healthily and lead active lifestyles.
The second participant stated they were liable for their choices, and no one else needed to hold them accountable. The third participant stated that their spouse and children supported their bariatric journey despite not being on the diet. The 10th participant persuaded a cousin to have bariatric surgery and occasionally shared recipes and ideas on maintaining healthy lifestyles. The fourth participant admitted they did not always “put in the work” to stay on task and confessed that finding excuses came easily. Nobody mentioned engaging in bariatric support groups, in person or online, or regular follow-ups with nutritionists, dietitians, or physicians. Batar et al10 suggested incorporating dietitians and behavioral and mental health counselors to encourage physical activity and enforce dietary modification to prevent weight gain.
Eating habits. Eating habits were associated with the participants’ behaviors when making healthy or unhealthy food choices. The data revealed that 100 percent of the participants understood the difference between making good or healthy food choices and bad or unhealthy food choices. All the participants understood the significance of meal preparation, drinking high-protein meal replacements, taking vitamins, and eating foods high in protein, nonstarchy vegetables, high-fiber grains, leafy greens, and healthy snacks. They also understood the importance of avoiding high-calorie foods, foods high in carbohydrates and saturated fats, refined starches, sweets, and sugary drinks, such as sweetened tea, sodas, and alcoholic beverages.
The first participant stated they usually ate vegetables, grilled or baked chicken, and grilled or baked pork chops as time permitted. However, they admitted they had not always made the best choices due to stress and family issues. The fifth participant shopped for Highkey products, a low-carb, healthier option compared to Oreo, Chips Ahoy, and other cookie brands. They also used Crystal Lite packets to flavor their water and drank Gold Peak Zero Sugar tea. When the third participant was busy or pressed for time, they went to places such as Chick-fil-a or Subway for healthy salad options. They opted for choices like vegetables, soup, and the salad bar in the cafeteria when they did not bring lunch and were the most adherent to healthy eating of all the participants.
Unfortunately, the participants made unhealthy choices during stressful situations; yielded to cravings, peer pressure, old habits; and ate comfort foods. The fourth participant said they started doing well with the diet but eventually returned to drinking sodas and sweet tea. That person grabbed whatever was quick and “knick-knacked” all day instead of eating balanced meals. The eighth participant acknowledged they skipped meals during busy times in their life. These findings suggest that early incorporation of an extensive support system that includes nutritionists and behavioral and mental health counselors could help participants stay on task and make healthy choices, especially during those challenging times.10
Physical activity. Physical activity is any human musculoskeletal system movement that generates energy expenditure during leisure time, walking, or occupation.11 For this investigation, physical activity can be viewed as going to the gym, participating in an exercise program, or engaging in any activity that requires increased physical moment. The study divided physical activity into two categories: active or inactive lifestyles. During the interviews, the participants were asked to rank their physical activity levels on the following scale: none, low, moderate, high, or extremely high. These data were not based on the frequency of exercise per week or the intensity of cardiopulmonary activity; it was an opportunity for personal reflection and self-reporting. Seventy-seven percent of the participants reported their physical activity levels as none, low, or moderate. No one felt their physical activity levels were high or extremely high. However, 100 percent of the participants admitted they could have done more to increase weight loss, such as exercising, increasing adherence to their diet, and keeping follow-up appointments with dietitians and physicians.
The third participant regularly enjoyed engaging in physical activities like walking, mobile application (app) workouts, going to the gym, and occasionally engaging with a personal trainer. That participant reported walking three miles 4 to 5 times a week, using a personal trainer for strength training, and engaging in 30-minute workouts using mobile apps when they could not go to the gym. Other participants considered going to work as their primary source of physical activity, regardless of the energy exerted to perform their job responsibilities; it did not matter whether the participants sat at a desk, walked in the hallways, or engaged in patient care—going to work was considered physical activity. The second participant stated they felt good about going to work after their procedure because they could get around easier without being in constant pain. That participant had the energy to run and play with their kids and engage in housework after working consecutive 12-hour shifts. That was impossible before bariatric surgery because of the weight, exhaustion, physical pain, and sedentary lifestyles.
The first participant found the gym intimidating and preferred activities like cleaning the house, doing laundry, going up and down the stairs, walking their dogs, and hanging out with family and friends. Spending time with family and friends included going to the park or community events that involved walking and being outdoors. A couple of participants did nothing outside of work. The sixth participant was a travel nurse with assignments out of town. On their off days, they wanted to relax with their kids, spouse, and dog and do nothing. This study indicates that patients need continued multidisciplinary support after bariatric surgery to initiate and maintain an active lifestyle.12
Mental and physical health. A mental health condition refers to a psychosocial issue diagnosed by a healthcare professional or self-diagnosis described by the participant. A self-diagnosis was strictly based on how the participant felt mentally or emotionally about having obesity. Mental health was divided into two categories, presence or absence of a mental health condition. Sixty-seven percent of the participants had a mental health diagnosis or experienced mental or emotional instability, potentially contributing to their obesity. The most common diagnoses of the participants included anxiety, depression, loneliness, panic attacks, and stress eating. All of these issues could affect adherence with staying on task with eating habits and engaging in physical activity.
The second participant said they had been diagnosed with anxiety and depression since the age of 16 years and struggled with being overweight for years. The third participant had difficulty moving away from their family and adjusting to a new location. The move proved emotionally challenging due to the lack of family support, distant friendships, and their spouse working many hours. The fifth participant disclosed that significant family events had led to an eating disorder, panic attacks, and depression. The only thing they felt they could control was food, which was the catalyst for their eating disorder. The seventh participant suffered verbal abuse during an unhealthy marriage centered on the inability to lose weight after having children. The eighth participant repressed their sexual orientation because of the “hillbilly” community they belonged to and the closed-minded people that surrounded them. All the participants stated that their mental health diagnoses or emotional state contributed to their obesity and was the root cause of their eating behaviors.
A physical health issue refers to a diagnosed or self-diagnosed medical condition of the body that lifestyles, behaviors, or unknown etiologies can cause. Physical health was divided into two categories, presence or absence of physical health challenges. Seventy-eight percent of the participants were diagnosed with or experienced physical health issues. Sleep apnea, hypertension, prediabetes, and elevated cholesterol were the most common physical health conditions. The first participant said they were diagnosed with sleep apnea, a thyroid condition, and polycystic ovary syndrome (PCOS). The thyroid condition and PCOS caused irregular hormone levels, menstruations, and weight gain.
The second participant was relieved to report they had only been diagnosed with hypertension but were on the verge of a prediabetes and hyperlipidemia diagnosis. The fifth participant had sleep apnea and alpha-thalassemia, a blood disorder that reduces the production of hemoglobin; elevated heart rate from physical activities caused them to pass out due to the limited oxygen-carrying capacity of their blood. The sixth participant reported having sleep apnea, but a family history of hypertension persuaded them to have bariatric surgery. The fourth participant had sleep apnea and osteoarthritis in both knees from being overweight. Both mental and physical health issues can lead to obesity and require more in-depth investigation and psychosocial support.
Health choices. The health choices section of the study determined whether the participants experienced any physical health advantages after having bariatric surgery, as well as barriers that prevented adherence to diet and physical activity. These health advantages included bariatric results, healthier eating habits, or active lifestyles. This section was divided into two categories: benefits and barriers. When comparing pre- and post-bariatric surgery weights, the participants lost between seven and 43 percent of their initial BMI, showing that bariatric surgery was advantageous. Aside from weight loss, the participants saw improvements in blood work values. The sixth participant said their hemoglobin A1c (HbA1c) and cholesterol levels improved, and their sleep apnea was resolved. The fifth participant stated they no longer took high blood pressure medicine, and their HbA1C was controlled. The first participant acknowledged taking a lower dose of thyroid medication after the weight loss. The fourth participant reported they did not experience any improvement in sleep or pain from osteoarthritis. That participant had the lowest weight loss and experienced weight gain postoperatively. While some health conditions improved after surgery among patients, there are no guarantees that the procedure will eliminate all health conditions.
The principal barriers that prevented the participants from consistently making good choices were lack of self-discipline, work schedules, and busy lifestyles. The ninth participant admitted that life was busy, and time prevented them from being more active. The second participant said work was their most significant barrier, especially working the night shift. Similarly, the fifth participant mentioned working irregular hours as a manager to meet staffing needs. Despite these challenges, the participants should incorporate healthy eating habits and physical activity into their daily schedules to eliminate barriers to making good decisions.
Self-image. Self-image refers to how participants perceived themselves and their feelings about the weight loss progress. This section was divided into three categories, positive, negative, or neutral states of mind. All the participants were extremely proud of their accomplishments of losing weight and planned to continue their bariatric journey. However, two participants expressed negative mental images of themselves, stating they still saw themselves as having morbid obesity. The first participant stated they still saw themselves as the “fat girl.” The eighth participant avoided walking through small spaces because they felt much larger. The ninth participant said they saw their self as the same size as before when looking in the mirror, despite going from 275 to 200 pounds. When they shopped, they selected the oversized clothing items they used to wear out of habit instead of the ones that were more size appropriate.
In contrast, some participants made positive affirmations of themselves. The third participant confessed that they saw their self in the same way because they never “picked (themselves) apart” before bariatric surgery; they always saw their self as a beautiful person. The fifth participant stated that they were “ridiculously happy and proud of themselves.” The weight loss validated their decision to have bariatric surgery. The sixth participant admitted they were always very confident, regardless of their weight. Self-perception could be the catalyst for continuously making healthy choices and engaging in active lifestyles to prevent weight regain.
Discussion
The sample population consisted of healthcare workers who had bariatric surgery at least one year prior to the time of the interview. The participants were motivated to have bariatric surgery for health reasons after years of failed diets, pain, discomfort, and medical conditions. However, after surgery, their motivation for eating healthy and engaging in physical activity was inconsistent and insufficient to keep them on task. Beltrán-Carrillo et al13 suggested a solid support system that included educational sessions with psychologists and dietitians for long-term lifestyle changes to help patients maintain healthy weights. The participants’ limited support systems could explain why they experienced weight regain.
Ben-Porat et al14 stated that bariatric patients who struggle with food addiction and binge eating learned to control their behaviors during the early postoperative phases because of their limited ability to intake food. The data revealed that the participants understood the importance of eating foods high in protein and nonstarchy vegetables and avoiding foods high in carbohydrates, saturated fats, and sugary drinks. However, they reverted to old eating behaviors, causing them to consume more calories than their dietary plans indicated. Similarly, González-Cutre et al15 indicated that bariatric patients who failed to engage in physical activity regularly or did not prioritize exercise in their lives were likely to experience weight regain. In this study, none of the participants reported being satisfied with their physical activity levels and stated they could have done more to increase weight loss. These findings confirm that the participants should engage in more physical activity to meet and maintain weight loss targets.
The study participants were diagnosed with mental health disorders that contributed to obesity and resulting physical health conditions. Gallé et al16 suggested that early implementation of multidisciplinary programs that include behavioral health services help bariatric patients establish healthy behaviors that last in the long-term. Issues such as depression, eating disorders, and body image obsessions require ongoing follow-up with behavioral health professionals.17 While some participants experienced health improvements and had medication dosages decreased, bariatric surgery is not guaranteed to eliminate all medical conditions. Osteoarthritis and alpha-thalassemia were the most restrictive diagnoses that prevented two participants from engaging in higher levels of physical activity, suggesting low-impact activities, including water aerobics, chair exercise, yoga, and pilates, should be considered.
Health choices highlighted the benefits and barriers to bariatric surgery in this study. The most significant advantage of having bariatric surgery was considerable weight reduction—16 to 186 pounds at the time of the interviews. While all the participants lost weight, they admitted they could have done more to increase their weight loss. They also reported improvements in blood pressure, cholesterol levels, and sleep. Wolfe et al18 showed that justification for bariatric surgery includes weight reduction, decrease in comorbidities, and better quality of life. Lack of self-discipline, busy work schedules, and demanding lifestyles among the patients prevented participants in the current study from consistently making good choices about healthy eating and engaging in physical activities. Billing-Bullen et al19 found that key barriers to a healthy lifestyle were food expenses, working hours, and cultural and social events centered on food, signifying the need for ongoing patient education and robust support systems facilitated by physicians, nurse practitioners, or dietitians.
Lastly, self-image highlighted how the patients perceived themselves and their weight loss. All the participants were proud of their weight loss accomplishment and vowed to continue pursuing their weight loss goals. However, some participants voiced negative mental images of themselves, indicating the need for ongoing psychosocial support after bariatric surgery.
Limitations and recommendations. The fundamental limitations of this study included sample size, limited diversity, time restraints, and data collection methods. The first limitation was a small sample size of participants that lacked diversity. This shortcoming was due to the population niche and limited accessibility of participants during the convenient sampling process. Future investigations should use scientific randomized sampling methods to capture a more diverse audience. Another limitation was that the researcher only used a questionnaire and interview questions they wrote to collect data due to institutional time restraints. Rewriting or using questions from existing studies could produce different results or identify new themes. Manipulating any of the limiting factors could expand the results of this investigation and extend its reach to a larger bariatric community.
Conclusion
The purpose of this research study was to evaluate how postoperative bariatric patients stay on task with nutrition goals and physical activity to prevent weight regain. Bariatric surgery was the most effective tool for weight loss and minimizing comorbidities, when combined with healthy eating and increased physical activity. Through thematic analysis and iterative comparison, the researcher identified several key themes, including motivation for surgery, support systems, eating habits, level of physical activity, mental health, physical health, health choices, and self-image, as variables that can be further explored. While adherence to nutritional and physical activity strategies was the best prognosis for long-term, postoperative weight loss, psychosocial and behavioral factors associated with obesity must also be considered.20 The data revealed that the participants who made unhealthy food choices and did not engage in physical activity regularly gained weight after surgery. The participants who were adherent to healthy eating habits or engaged in low-to-moderate impact physical activity (Participants 3, 7, and 9) did not experience weight regain. While the third participant was the most adherent to diet and exercise, the seventh and ninth participants were relatively new to the bariatric journey and focused more on diet than exercise. Bariatric surgery must be perceived as a lifelong journey to experience lasting results motivated by intrinsic and extrinsic factors.
References
- American Society for Metabolic and Bariatric Surgery. Metabolic and bariatric surgery. Jul 2021. https://asmbs.org/resources/metabolic-and-bariatric-surgery. Accessed 9 Jan 2023.
- World Health Organization. Obesity and overweight. 9 Jun 2021. https://www.who.int/news-room/fact-sheets/detail/obesity-and-overweight. Accessed 9 Jan 2023.
- Mayo Clinic. Weight regain after bariatric surgery. 13 Jun 2018. https://www.mayoclinic.org/medical-professionals/endocrinology/news/weight-regain-after-bariatric-surgery/mac-20431467. Accessed 9 Jan 2023.
- Arterburn DE, Telem DA, Kushner RF, Courcoulas AP. Benefits and risks of bariatric surgery in adults: a review. JAMA. 2022;324(9):879–887.
- Therrien S, Simonetti J. Obesity medicine and a call to action: weight recidivism post weight loss surgery and the argument for mandatory medical weight management as a postoperative standard within bariatric surgery practices. Bariatric Times. 2020;17(8):10–11.
- Leedy PD, Ormrod JE. Practical research: Planning and Design, 9th ed. Pearson Education, Inc.; 2010.
- Centers for Disease Control and Prevention. About adult BMI. Reviewed 3 Jun 2022. https://www.cdc.gov/healthyweight/assessing/bmi/adult_bmi/index.html. Accessed 9 Jan 2023.
- Asbjørnsen R, Wentzel J, Smedsrød M, et al. Identifying persuasive design principles and behavior change techniques supporting end user values and needs in eHealth interventions for long-term weight loss maintenance: qualitative study. J Med Internet Res. 2020;22(11):e22598.
- Robinson A, Husband A, Slight R, Slight S. Digital support for patients undergoing bariatric surgery: narrative review of the roles and challenges of online forums. JMIR Perioper Med. 2020;3(2):e17230.
- Batar N, Kermen S, Sevdin S, Coşkun H, et al. Assessment of the correlation between weight status and the frequency of dietician interviews in sleeve gastrectomy patients. Obes Surg. 2021;31(1):185–193.
- World Health Organization. Physical activity fact sheet. 2021. https://apps.who.int/iris/bitstream/handle/10665/346252/WHO-HEP-HPR-RUN-2021.2-eng.pdf?sequence=1. Accessed 9 Jan 2023.
- Tullberg HS, Olsén MF, Shams K, Wiklund M. “Stepping with ease towards a new way of living”– experiences of physical activity 5 years after bariatric surgery. Eur J Physiother. 2017;19(3):154–159.
- Beltrán-Carrillo VJ, Jiménez-Loaisa A, Jennings G, et al. Exploring the socio-ecological factors behind the (in)active lifestyles of Spanish post-bariatric surgery patients. Int J Qual Stud Health Well-being. 2019;14(1):1626180.
- Ben-Porat T, Košir U, Peretz S, et al. Food addition and binge eating impact on weight loss outcomes two years following sleeve gastrectomy surgery. Obes Surg. 2022;32(4):1193–1200.
- González-Cutre D, Jiménez-Loaisa A, Alcaraz-Ibáñez M, et al. Motivation and physical activity levels in bariatric patients involved in a self-determination theory-based physical activity program. Psychol Sport Exerc. 2020;51:101795.
- Gallé F, Marte G, Cirella A, et al. An exercise-based educational and motivational intervention after surgery can improve behaviors, physical fitness, and quality of life in bariatric patients. PLoS ONE. 2020;15(10):e0241336.
- Jumbe S, Hamlet C, Meyrick J. Psychological aspects of bariatric surgery as a treatment for obesity. Curr Obes Rep. 2017;6(1):71–78.
- Wolfe BM, Kvach E, Eckel RH. Treatment of obesity: weight loss and bariatric surgery. Circ Res. 2016;118(11):1844–1855.
- Billing-Bullen G, Nielsen D, Wham C, Kruger R. Enablers and barriers to prevent weight-regain post bariatric surgery – a qualitative enquiry. Eat Behav. 2022;47:101677.
- Cadena-Obando D, Ramírez-Rentería C, Ferreira-Hermosillo A, et al. Are there really any predictive factors for a successful weight loss after bariatric surgery? BMC Endocr Disord. 2020;20(1):20.
Category: Current Issue, Original Research




