Normative Data for the Brief Symptom Inventory in a Bariatric Surgery-seeking Patient Sample

by Jeremy E. Mirsky, PhD, ABPP
Dr. Mirsky is with Massachusetts General Brigham Integrated Care in Watertown, Massachusetts.
Funding: No funding was provided for this article.
Disclosures: The author has no conflicts of interest relevant to this article.
Bariatric Times. 2023;20(1):11–15.
Abstract
Objective: Previous literature has suggested that between 50 and 66 percent of bariatric surgery clinics use an objective psychometric instrument as part of the presurgical evaluation. Normative scores for bariatric populations are often higher than those for populations without obesity. The Brief Symptom Inventory (BSI) has been used in previous research with bariatric populations, but no normative data have been reported in the literature. The present study provides a set of normative data for the BSI in a bariatric population, in addition to data on internal consistency reliability. It was hypothesized that subscale and index scores would be significantly greater for bariatric patients relative to the original, nonclinical normative sample.
Design: BSI protocols for 658 presurgical patients were extracted from archival clinic data. Subscale scores were calculated, and t-tests were conducted to check for differences between mean scores among bariatric patients and a nonclinical sample.
Setting: The study took place at an outpatient behavioral medicine department of a large, multispecialty medical practice in Central Massachusetts.
Participants: The sample consisted primarily of women (80%), with a mean age of 45.41±12.23 years and a mean body mass index (BMI) of 46.51±7.83kg/m2.
Results: Consistent with the study hypothesis, BSI subscale scores (with one exception) and indices were higher for bariatric patients than for nonclinical individuals, supporting the need for bariatric-specific norms. Reliability coefficients were satisfactory for all but one subscale.
Conclusion: These data provide clinicians and researchers with an appropriate set of norms for the BSI when used with patients who are seeking bariatric surgery.
Keywords: Brief Symptom Inventory, BSI, psychological evaluation, psychopathology, test norms
Psychologists and other mental health practitioners differ widely in their strategies for assessing potential bariatric surgery candidates. Previous reports have indicated that between 50 and 66 percent of bariatric surgery clinics reported using an objective psychometric instrument as part of the presurgical evaluation.1,2 A recent review of self-report psychological measures used in bariatric evaluations3 included the Symptom Checklist-90 Revised (SCL-90-R),4 but not the Brief Symptom Inventory (BSI),5 which is a shorter form adapted from the SCL-90. Ransom et al6 examined the use of the SCL-90-R with bariatric surgery candidates and reported internal consistency coefficients ranging from 0.76 to 0.90 for the subscales and some evidence of convergent validity.
The BSI is a 53-item self-report inventory that assesses a broad range of psychiatric symptomatology. The BSI was initially normalized on psychiatric inpatients, psychiatric outpatients, and nonclinical individuals. The adult nonclinical normative sample for the BSI (n=974) consisted of 50.7 percent men and 49.3 percent women, with a mean age of 46.0 years (standard deviation [SD]: 14.7). Given that the BSI was not developed in the context of weight-related concerns, there are no body mass index (BMI) data for the sample. The BSI has nine subscales: somatization (SOM), depression (DEP), phobic anxiety (PHO), obsessive compulsive (OC), interpersonal sensitivity (IS), anxiety (ANX), paranoia (PAR), psychoticism (PSY), and hostility (HOS). Items are rated on a 5-point scale ranging from 0 (“not at all”) to 4 (“extremely”). In addition, there are three index scores: the Global Severity Index (GSI), Positive Symptoms Total (PST), and Positive Symptom Distress Index (PSDI). The GSI is essentially the mean of all subscale scores. The PST is the total of items endorsed with a response greater than zero (i.e., indicating self-reported presence of the symptom). The PSDI is the quotient of total item values divided by the PST. The BSI administration time is estimated to be between 8 and 10 minutes.5
The BSI has been used in published studies with various medical populations (e.g., traumatic brain injury, cancer survivors, cardiac failure, renal dysfunction, breast cancer). Psychometric properties of a tool are population-specific; that is to say, while a psychological measure might possess acceptable reliability and validity coefficients with one population, it might not in another. Walfish et al7 found that half of the subscales of the Millon Behavioral Medicine Diagnostic (MBMD)8 lacked acceptable reliability coefficients in a sample of bariatric surgery patients. Similarly, recommended cutoff scores for one population might not apply to another. For example, based on empirical analysis, Cassin et al9 recommended a cutoff score of 15, as opposed to the commonly used cutoff score of 10, on the Patient Health Questionnaire-9 (PHQ-9)10 depression screen when used with bariatric surgery candidates. Psychiatric symptom inventories often include questions that load heavily on somatic complaints, which might be normatively higher in individuals with various medical conditions (e.g., obesity, chronic pain, multiple sclerosis), independent of psychiatric symptoms or disorder.
To date, there have been no psychometric normative data reported on the use of the BSI in patients seeking bariatric surgery for morbid obesity. The GSI of the BSI was utilized to investigate obesity stigmatization and coping in a sample that included 77 percent gastric bypass patients; however, normative psychometric data were not provided.11 Friedman et al12 only reported on the GSI for patients who were attending a residential program for nonsurgical weight loss. In that study, the means and SDs were reported separately for male patients (mean: 0.74, SD: 0.53) and female patients (mean: 0.80, SD: 0.53).12 Odom et al13 used the BSI-18, an 18-item short form, in their study of behavioral predictors of weight regain after bariatric surgery, but they did not report the descriptive statistics of the measure.
Individuals seeking bariatric surgery have higher lifetime and current rates of psychiatric disorders than the general population.14 Individuals with obesity face widespread stigmatization and discrimination.12,15,16 Taken together, it is reasonable to believe that BSI subscales assessing depression, anxiety, paranoia, phobic anxiety, and interpersonal sensitivity might be elevated among individuals seeking bariatric surgery. This idea is supported by several studies of Minnesota Multiphasic Inventory 2 (MMPI-2)17 profiles of bariatric surgery candidates.
The MMPI-2 is a widely used, standardized 567-item test that assesses personality traits and psychopathology. Considered a broad band instrument, the MMPI-2 contains 10 clinical scales which cover a range of concerns (e.g., depression, somatization, social adjustment, interpersonal sensitivity, paranoia). The MMPI-2 has been extensively used in research with medical populations including bariatric patients. Maddi et al18 examined MMPI-2 profiles in a large sample (n=1,027) of bariatric surgery patients. These investigators found elevations (defined as t-scores ≥65) on all scales, with the exceptions of scales 5 (“Masculinity/Femininity”) and 9 (“Hypomania”).18 Some of the clinical scales that were elevated contain items that relate, in part, to paranoia, social alienation, and social introversion/interpersonal sensitivity. These scales might tap some of the experiences of stigmatized individuals. Kinder et al19 reported similar results.
Reliance on existing BSI norms can result in overestimates of psychopathology in patients seeking bariatric surgery. The aim of the current study was to provide a set of normative data for the BSI based on a pre-bariatric surgery population. It was hypothesized that mean scores for all BSI subscales and indices would be significantly higher in the bariatric sample than in the original, nonclinical normative sample.5
Methods
Procedure. Archival data from a bariatric behavioral medicine clinic were used for the current analyses. Patients in the bariatric program completed the BSI on the same day that they began a required six-week presurgical treatment based on cognitive-behavioral principles. Completion of the BSI occurred after the initial clinical evaluation. The study was deemed exempt by the organization’s Institutional Review Board (IRB). Furthermore, patients in the program provided informed consent that their data may be used in aggregate form for program evaluation and/or research purposes
Sample. The sample included 658 patients who were evaluated by psychologists in the behavioral medicine clinic as part of the bariatric surgery program. All patients were presurgical. Exclusionary criteria for the group treatment included active and untreated psychosis, active suicidality, active substance abuse, psychiatric hospitalization within the past 12 months, and active purging behaviors. While a diagnostic evaluation was conducted for each patient, clinical diagnoses were not included in the data set used for this study.
Data analysis. The BSI subscale and global index scores were calculated based on the formulae presented in the BSI manual. Complete data were available for 658 patients. Means and SDs were calculated for each of the BSI subscales and indices. Welch’s t-tests were used to compare mean scores on all subscales and indices between the bariatric sample and Derogatis’s nonclinical normative sample. Welch’s t-tests were chosen because they do not require the assumption of equal variances in the two groups. Two-sample t-tests were used to assess for sex differences within the bariatric sample.
Results
Participants were between the ages of 18 and 80 years, with a mean age of 45.41±12.23 years. Eighty percent of the participants were female (n=529), and the remaining 20 percent were male (n=129). This ratio is reflective of the overall sex disparity seen in our bariatric clinic, which is consistent with that of Fuchs et al,20 who found that approximately 80 percent of individuals who undergo bariatric surgery are female. The mean BMI for the entire sample was 46.51±7.83kg/m2, with a range of 29.92 to 92.24kg/m2.
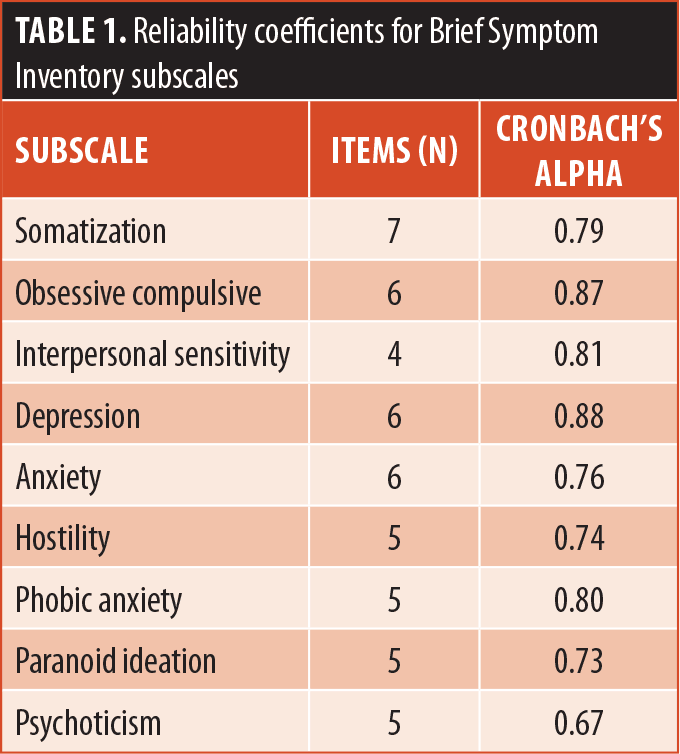
Internal consistency. Coefficient alphas ranged from 0.67 to 0.88 (Table 1). All but one of the subscales had a Cronbach’s coefficient alpha of at least 0.73. These reliability coefficients are considered satisfactory by conventional standards. The exception was the PSY subscale, which had an alpha of 0.67.
Normative data. Means and SDs for each of the BSI subscales and global indices appear in Table 2. Table 3 displays comparisons of the means and SDs from the current sample with those reported by Derogatis for his sample of nonclinical adults. Statistically significant differences were found for all subscales and indices except HOS, with bariatric patients scoring higher than the nonclinical sample on each, as predicted.
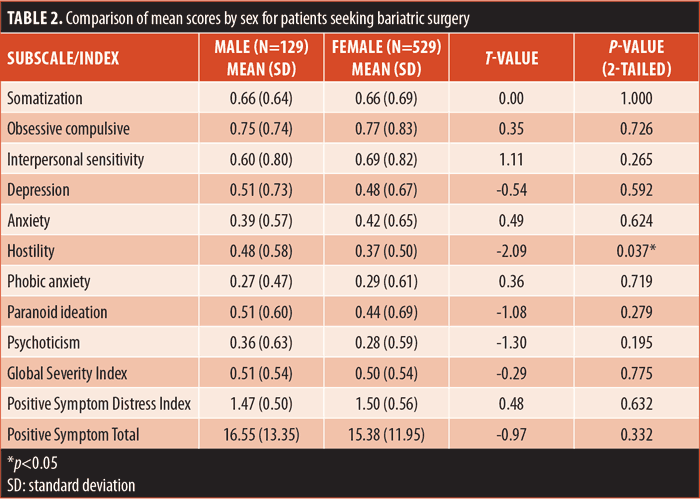
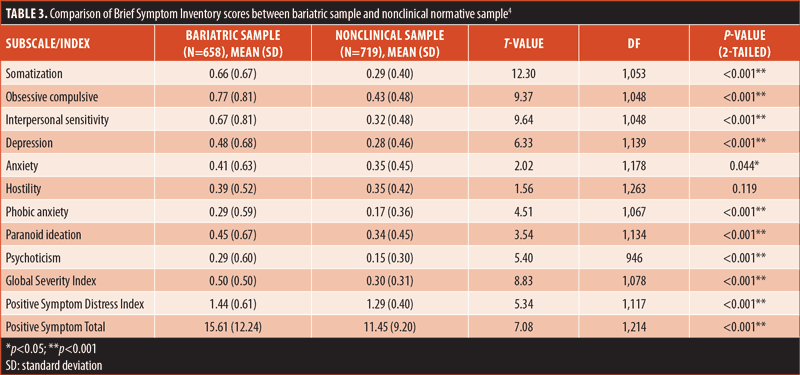
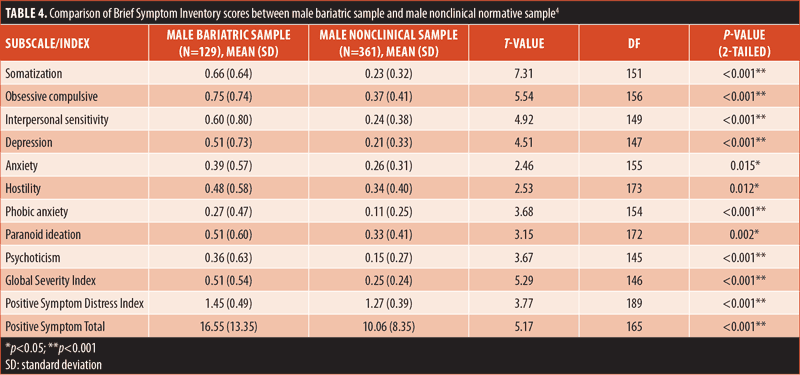
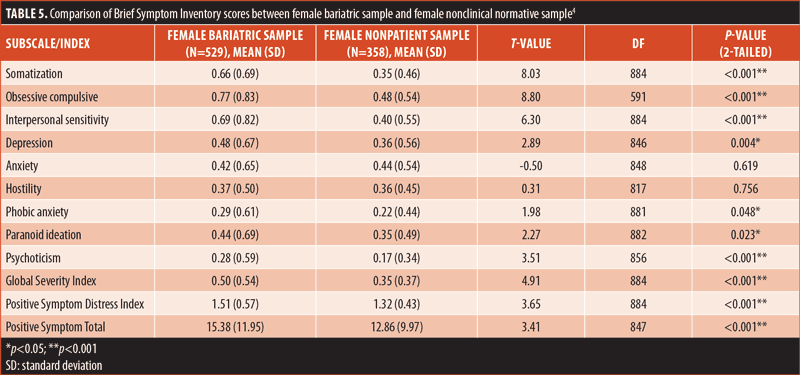
Sex comparisons. Additional t-tests were calculated to determine whether there were significant sex differences. The only significant sex difference found among the bariatric sample was on the HOS subscale, on which male patients scored higher than female patients (t=2.53, p=0.01). Tables 4 and 5 present the comparisons between bariatric and nonclinical individuals among male and female individuals, respectively. When compared to Derogatis’s nonclinical sample, it was found that male patients in the bariatric sample scored significantly higher on the HOS subscale (t=2.53, p=0.01), while female patients did not. Male patients in the bariatric sample scored significantly higher on all subscales and indices than nonclinical male individuals. Female patients in the bariatric sample scored significantly higher on all subscales and indices than did nonclinical female individuals, with the exception of the ANX and HOS subscales, for which there were no statistically significant differences.
Discussion
Results largely supported the hypothesis that BSI subscale scores and indices would be higher in the bariatric sample than in the nonclinical sample reported in the BSI test manual. All subscale and index scores except for HOS (i.e., SOM, OC, IS, DEP, ANX, PHO, PAR, PSY) were higher. There was no statistically significant difference on the HOS subscale.
Internal consistency coefficients for all subscales were satisfactory (i.e., ≥0.70), with the exception of PSY. Similarly, Derogatis reported the PSY coefficient alpha (0.71) to be the lowest of the subscales in a sample of 719 psychiatric outpatients.4 Terascavage et al21 noted a low reliability coefficient on MMPI-2 Restructured Form thought dysfunction scale in a bariatric sample and suggested that this was due to restriction in range, given the low base rate in this population. However, Derogatis’s reliability coefficient was based on a sample of psychiatric outpatients, in which thought dysfunction has a relatively higher base rate.
The higher subscale scores do not necessarily indicate greater psychopathology among patients seeking bariatric surgery. It is possible that the higher scores are reflective of “demoralization saturation” (i.e., overall emotional discomfort not specific to each subscale), as has been reported with the MMPI-2.22 Even if that is the case, it is still important to take these higher scores into account, lest the level of symptomatology be overestimated. At the same time, that would call into question the discriminant validity of the BSI when used in bariatric patient populations
Limitations. One limitation of the current study is that diagnostic information was not available in the data set, and therefore the sample could not be divided based on presence or absence of psychiatric diagnosis. A second limitation is the fact that the sample is limited to those patients who were deemed to be appropriate candidates to begin the bariatric treatment program (e.g., cognitive-behavioral group treatment, consultations with dietitians), although no patients in the program were cleared for surgery at the outset. A very small minority of patients seen for initial evaluation might not have been referred to the group (and therefore not included in the study) due to clinician judgment that they were not suitable candidates for the group at the time (e.g., due to untreated, significant, severe psychopathology, or active substance abuse). Therefore, these BSI data might not reflect the full range of psychopathology for patients who have presented for evaluation (e.g., individuals with untreated psychosis or significant substance abuse). However, given that the number of patients who are not allowed entry into the program is very low, any restriction in range is likely negligible, and offset by the large sample size.
Another limitation is the lack of sociodemographic data regarding the sample. Inclusion of ethnicity, relationship status, level of education, and employment status, among others, can help clinicians and researchers determine whether the study participants are a representative sample of the target population for purposes of generalization. Furthermore, incorporation of such variables can be a step toward building studies that better reflect the range of societal diversity.
Conclusion
These data provide clinicians and researchers with an appropriate set of norms for the BSI when used with patients seeking bariatric surgery. Use of inappropriate test norms can lead to overestimation or underestimation of psychopathology. It is recommended that clinicians utilize bariatric-specific normative data when employing the BSI with this patient population, unless the use of psychiatric patient norms is more appropriate for the specific patient.
While the current study provides normative data, it does not establish predictive or convergent validity for the BSI. Future research should investigate validity through the use of external criteria, as well as sensitivity to change in a bariatric population. Research investigating discriminant validity could be useful in determining whether the BSI is reflecting an overall demoralization factor in this population or whether the factors underlying the subscales provide unique information.
References
- Fabricatore AN, Crerand CE, Wadden TA, et al. How do mental health professionals evaluate candidates for bariatric surgery? Survey results. Obes Surg. 2006;16(5):567–573.
- Bauchowitz AU, Gonder-Frederick LA, Olbrisch ME, et al. Psychosocial evaluation of bariatric surgery candidates: a survey of present practices. Psychosom Med. 2005;67(5):825–832.
- Marek RJ, Heinberg LJ, Lavery M, et al. A review of psychological assessment instruments for use in bariatric surgery evaluations. Psychol Assess. 2016;28(9):1142–1157.
- Derogatis LR. SCL-90-R. Administration, Scoring, and Procedures Manual for the Revised Version of the SCL-90. John Hopkins University Press; 1977.
- Derogatis LR. BSI: Brief Symptom Inventory. National Computer Systems; 1993.
- Ransom D, Ashton K, Windover A, Heinberg L. Internal consistency and validity assessment of SCL-90-R for bariatric surgery candidates. Surg Obes Relat Dis. 2010;6(6):622–627.
- Walfish S, Wise EA, Streiner DL. Limitations of the Millon Behavioral Medicine Diagnostic (MBMD) with bariatric surgical candidates. Obes Surg. 2008;18(10):1318–1322.
- Millon T, Antoni M, Millon C, Grossman S. Millon Behavioral Medicine Diagnostic. NCS Assessments; 2001.
- Cassin S, Sockalingam S, Hawa R, et al. Psychometric properties of the patient health questionnaire (PHQ-9) as a depression screening tool for bariatric surgery candidates. Psychosomatics. 2013;54(4):352–358.
- Kroenke K, Spitzer RL, Williams JB. The PHQ-9: validity of a brief depression severity measure. J Gen Intern Med. 2001;16(9):606–613.
- Myers A, Rosen JC. Obesity stigmatization and coping: relation to mental health symptoms, body image, and self-esteem. Int J Obes Relat Metab Disord. 1999;23(3):221–230.
- Friedman KE, Reichmann SK, Costanzo PR, et al. Weight stigmatization and ideological beliefs: relation to psychological functioning in obese adults. Obes Res. 2005;13(5):907–916.
- Odom J, Zalesin KC, Washington TL, et al. Behavioral predictors of weight regain after bariatric surgery. Obes Surg. 2010;20(3):349–356.
- Malik S, Mitchell JE, Engel S, et al. Psychopathology in bariatric surgery candidates: a review of studies using structured diagnostic interviews. Compr Psychiatry. 2014;55(2):248–259.
- Puhl R, Brownell KD. Bias, discrimination, and obesity. Obes Res. 2001;9(12):788–805.
- Spahlholz J, Baer N, König HH, et al. Obesity and discrimination – a systematic review and meta-analysis of observational studies. Obes Rev. 2016;17(1):43–55.
- Butcher, JN, Graham, JR, Ben-Porath, YS. Minnesota Multiphasic Personality Inventory–2 (MMPI-2): Manual for Administration and Scoring. University of Minnesota Press; 1995.
- Maddi SR, Khoshaba DM, Persico M, et al. Psychosocial correlates of psychopathology in a national sample of the morbidly obese. Obes Surg. 1997;7(5):397–404.
- Kinder BN, Walfish S, Scott Young M, Fairweather A. MMPI-2 profiles of bariatric surgery patients: a replication and extension. Obes Surg. 2008;18(9):1170–1179.
- Fuchs HF, Broderick RC, Harnsberger CR, et al. Benefits of bariatric surgery do not reach obese men. J Laparoendosc Adv Surg Tech A. 2015;25(3):196–201.
- Tarescavage AM, Wygant DB, Boutacoff LI, Ben-Porath YS. Reliability, validity, and utility of the Minnesota Multiphasic Personality Inventory-2-Restructured Form (MMPI-2-RF) in of bariatric surgery candidates. Psychol Assess. 2013;25(4);1179–1194.
- Tellegen A, Ben-Porath YS, McNulty JL, et al. MMPI-2 Restructured Clinical (RC) Scales: Development, Validation, and Interpretation. University of Minnesota Press; 2003.
Category: Original Research, Past Articles




