Raising the Standard: Healthcare Worker Wellbeing During COVID-19: The State of The Literature: Part 1

by Kristen Demertzis, PhD, ABPP-CN; Rebecca M. Schwartz, PhD; and Dominick Gadaleta, MD, FACS, FASMBS
Dr. Demertzis is the Chief of Neuropsychology at South Shore University Hospital and the Director of Resident and Fellow Mentorship and Faculty Development for Northwell Health’s OB/GYN Departments at South Shore University Hospital and Huntington Hospital; Assistant Professor of Physical Medicine and Rehabilitation and of Psychiatry at the Zucker School of Medicine at Hofstra/Northwell in Hempstead, New York. Dr. Schwartz is Director of Research and Evaluation for Northwell Health’s Center for Traumatic Stress, Resilience and Recovery; Chief of Social Behavioral Sciences and an Associate Professor of Occupational Medicine, Epidemiology, and Prevention at the Zucker School of Medicine at Hofstra/Northwell in Hempstead, New York; Associate Investigator at Northwell’s Feinstein Institutes for Medical Research. Dr. Gadaleta is Chair, Department of Surgery, South Shore University Hospital; Director, Metabolic and Bariatric Surgery, North Shore and South Shore University Hospitals, Northwell Health in Manhasset, New York; Associate Professor of Surgery, Zucker School of Medicine at Hofstra/Northwell in Hempstead, New York.
Funding: No funding was provided for this article.
Disclosures: The authors report no conflicts of interest relevant to the content of this article.
Bariatric Times. 2022;19(3):14–15
This is Part 1 of a two-part series that examines the wellbeing of healthcare workers surrounding the COVID-19 pandemic.
Mental health concerns and burnout affect a substantial percentage of healthcare workers (HCWs) and have been associated with substance abuse, decreased quality of life, and suicide.1–4 Occupational impacts include, but are not limited to, poorer patient safety and quality outcomes and lower job satisfaction, retention, and productivity.3–7 Epidemics adversely impact mental health and burnout rates among HCWs.8 With over 357 million COVID-19 cases and over 5.5 million COVID-19-related deaths recorded in the United States (US) as of January 2022,9 the pandemic’s toll on the wellbeing of HCWs has been significant and, in some cases, has tragically led to suicide.10,11
Multiple COVID-19-related studies have reported elevated anxiety, depressive symptoms, posttraumatic stress symptoms, burnout, moral injury, and suicidal ideation among HCWs.9,12–15 Factors associated with poorer outcomes include female sex, graduate medical trainee/early career status, high-exposure work settings, redeployment (particularly outside of expertise), overextended work hours, quarantining/interpersonal isolation, contracting COVID-19, dissatisfaction with organizational support (e.g., availability of personal protective equipment [PPE], testing, or childcare), life-and-death patient care determinations amid surged hospitalizations and limited resources, pre-existing burnout, greater childcare/schooling/household responsibilities, and maladaptive coping styles (e.g., avoidance, self-blame).9,13,16–24 With a historical precedent for increased minority scapegoating during epidemics and pandemics25 and seven percent of US HCWs self-identifying as Asian,26 HCWs’ wellbeing have also suffered secondary to pandemic-heightened xenophobia and anti-Asian sentiment.27,28
Some protective factors during this and other severe acute respiratory syndrome (SARS) outbreaks include access to social support, perceived adequacy of training, sufficient medical resources, up-to-date and accurate information with clear communication of directives and precautionary measures, organizational responsiveness and support, and adaptive coping strategies (e.g., problem solving, humor).29–32 Listening sessions with multidisciplinary HCWs early in the pandemic revealed the following themes: hear me, protect me, prepare me, support me, care for me, and honor me.33
The nature and drivers of mental health outcomes have been examined over time to understand intricacies of the pandemic’s impact. One study surveyed HCWs (n=1831) in April/May 2020 (Phase 1) and October/November 2020 (Phase 2).34 Phase 1 results revealed significant fear about catching/spreading COVID-19, uncertainty about COVID-19 and its societal repercussions, and concern about frequent protocol changes and PPE reliability and availability. Phase 2 results demonstrated decreased fear given increased virus knowledge, greater PPE availability, and more established protocols, but prominent presence of exhaustion or “COVID fatigue.” Feelings of isolation and loneliness spanned both phases. Though technology (e.g., telehealth, virtual meetings) had a beneficial impact, HCWs also noted negative aspects to virtual interactions (e.g., characterizing them as “completely unrewarding” and “dehumanizing and disjointed”).34
Some studies show promising trends of decreasing levels of stress and depressive, anxiety, and posttraumatic stress symptoms.29 Other studies show that even when community infection rates and hospital admissions are down, HCWs are feeling devalued and emotionally drained amid continued demanding work schedules and staff challenges.35 A repeated cross-sectional study of intensivists, for instance, revealed increased workload, professional/personal isolation, and compassion fatigue and reduced physical activity from spring 2020 to spring 2021.36 Occupational stress was associated with elevated emotional distress, burnout, and intention to quit. Data from this and prior epidemics/pandemics underscore the importance of continued wellbeing surveillance in HCWs to best understand their experiences, factors heightening or mitigating risk for poor outcomes, and effective interventions.
Northwell Employee Wellbeing Research Consortium Registry
To this end, Northwell Health established an interdepartmental, multidisciplinary Employee Wellbeing Research Consortium in an effort to characterize the pandemic’s impact on the mental health and wellbeing of HCWs. The Consortium received Institutional Review Board (IRB) approval in June 2020 to initiate a research registry that follows cohorts of HCWs over time. The registry’s goals are two-fold: 1) to further the science of occupational health and wellness during the pandemic using cross-sectional and longitudinal data to elucidate factors that place HCWs at risk for poor mental health and wellbeing and elucidate factors associated with resilience and 2) to use survey data to guide leadership, department/division chairs, training program directors, and other clinical leaders as to what policies/procedures support the wellbeing of HCWs and what factors might increase the risk of stress, burnout, and poor mental health.
Two cohorts have been established thus far: physicians and nurses/nursing staff. A secure, Health Insurance Portability and Accountability Act of 1996 (HIPAA)-compliant database, Research Electronic Data Capture (REDCap), is used for all consent, baseline, and follow-up data collection purposes. Physicians and nursing staff actively employed by or affiliated with the hospital system are eligible for study inclusion. Baseline assessments were completed between June and August 2020, and follow-up surveys are automatically sent to participants every six months thereafter for five years. The total baseline sample was 620 physicians and 871 nurses/nursing staff.
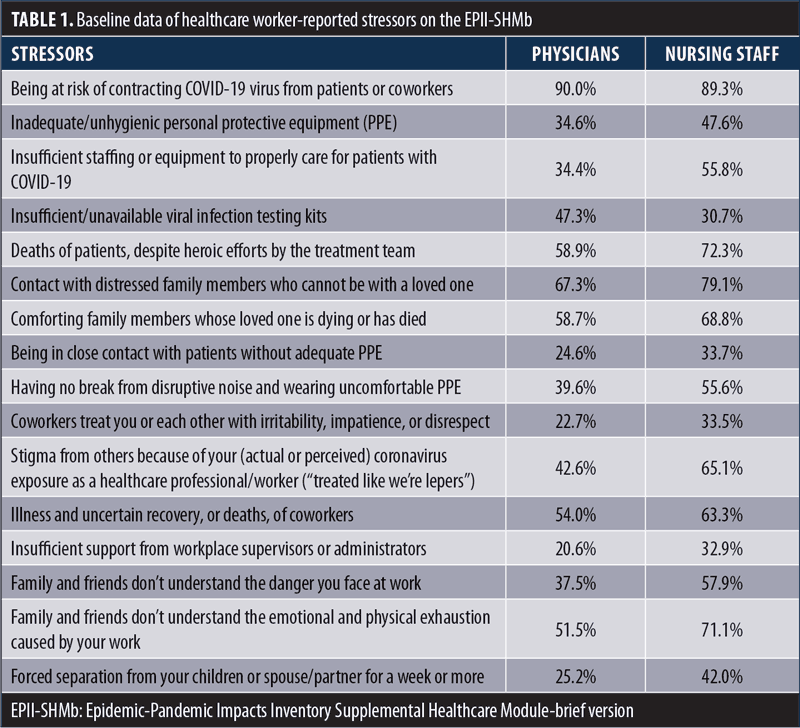
Table 1 presents baseline data from the Epidemic-Pandemic Impacts Inventory Supplemental Healthcare Module-brief version (EPII-SHMb),37 which represents self-reported stressors experienced since the start of the pandemic. Consistent with extant COVID-19 literature, the top three stressors reported by both physicians and nurses/nursing staff were risk of contracting COVID-19 from patients/coworkers, contact with distressed family members who cannot be with a loved one, and deaths of patients, despite heroic efforts by the treatment team.
Over 25 percent of nurses/nursing staff and almost 15 percent of physicians responded “definitely” to feeling unprepared for the moral dilemma of having to deny lifesaving treatment due to shortages or rationing.38 On the positive side, higher levels of resilience were demonstrated, as over 53 percent of physicians and 58 percent of nurses/nursing staff indicated “definitely” to feeling proud about what they have accomplished at work, and over 50 percent of both groups indicated “definitely” feeling as though they have made an important difference in patients’ lives.38
Thus far, a number of publications and abstracts are in progress or have been published using data from the Employee Well-being Research Consortium registry. One such manuscript recently has been published in the Journal of Occupational and Environmental Medicine.18 Multivariable model analyses of baseline data revealed that with each additional negative occupational experience reported by physicians on the EPII-SHMb items listed in Table 1, there was a 23-percent increased odds of probable anxiety and depression and a 41-percent increased odds of probable posttraumatic stress disorder (PTSD). Conversely, higher levels of self-perceived resilience consistently reduced the odds of anxiety, depression, and PTSD, and higher levels of perceived occupational support were associated with decreased odds of probable anxiety. Similarly, in another study recently published by the consortium researchers in Archives of Environmental and Occupational Health, redeployment and trainee status were specifically examined as they relate to aspects of burnout.12 Physician redeployment was associated with a 53-percent increased odds of emotional exhaustion, which is a key aspect of burnout, and trainee status (i.e., resident or fellow) was associated with a 59-percent increased odds of emotional exhaustion.
Conclusion
These studies underscore the impact that pandemic occupational experiences have on the wellbeing of HCWs and that specific groups (e.g., trainees) might be at heightened risk for adverse effects, such as burnout. Results are also consistent with models of clinician burnout and wellbeing,4,39 in that there are numerous, multi-level factors that can directly impact or modify negative effects on the wellbeing of HCWs. Findings elucidate the need for mental health support resources and policies to address structural issues at all levels (e.g., staffing, PPE access, childcare coverage) to maximize wellbeing for the healthcare workforce, particularly during this time. In next month’s column, we will review the literature and discuss specific resources surrounding supporting the wellbeing of HCWs during the COVID-19 pandemic.
References
- Dyrbye LN, West CP, Satele D. Burnout among U.S. medical students, residents, and early career physicians relative to the general U.S. population. Acad Med. 2014;89:443–451.
- Woo T, Ho R, Tang A, Tam W. Global prevalence of burnout symptoms among nurses: a systematic review and meta-analysis. J Psychiatr Res. 2020;123:9–20.
- Mihailescu M, Neiterman E. A scoping review of the literature on the current mental health status of physicians and physicians-in-training in North America. BMC Public Health. 2019;19(1):1363.
- Shanafelt TD, Noseworthy JH. Executive leadership and physician well-being: nine organizational strategies to promote engagement and reduce burnout. Mayo Clin Proc. 2017;92(1):129–146.
- Dall’Ora C, Ball J, Reinius M, Griffiths P. Burnout in nursing: a theoretical review. Hum Resour Health. 2020;18(1):41.
- Halbesleben JRB, Rathert C. Linking physician burnout and patient outcomes: exploring the dyadic relationship between physicians and patients. Health Care Manage Rev. 2008;33(1):29–39.
- Panagioti M, Geraghty K, Johnson J. Association between physician burnout and patient safety, professionalism, and patient satisfaction: a systematic review and meta-analysis. JAMA Intern Med. 2018;178:1317–1331.
- Chigwedere OC, Sadath A, Kabir Z, Arensman E. The impact of epidemics and pandemics on the mental health of healthcare workers: a systematic review. Int J Environ Res Public Health. 2021;18(13):6695.
- John Hopkins University and Medicine Coronavirus Resource Center. Tracked reported cases of COVID-19. Updated 25 Jan 2022. https://coronavirus.jhu.edu/map.html. Accessed 25 Jan 2022.
- Linzer M, Stillman M, Brown R, et al. Preliminary report: US physician stress during the early days of the COVID-19 pandemic. Mayo Clin Proc Innov Qual Outcomes. 2021;5:127–136.
- Knoll C, Watkins A, Rothfeld M. “I couldn’t do anything:” the virus and an E.R. doctor’s suicide. NY Times. 11 Jul 2020. https://www.nytimes.com/2020/07/11/nyregion/ lorna-breen-suicide-coronavirus.html. Accessed 25 Jan 2022.
- Singh V, Young J, Malhotra P, et al. Evaluating burnout during the COVID-19 pandemic among physicians in a large health system in New York. [published online ahead of print, 8 Jan 2022] Arch Environ Occup Health. 2022;1–9.
- Vizheh M, Qorbani M, Arzaghi SM, et al. The mental health of healthcare workers in the COVID-19 pandemic: a systematic review [published online ahead of print, 26 Oct 2020]. J Diabetes Metab Disord. 2020;19(2):1–12.
- Kok N, van Gurp J, Teerenstra S, et al. Coronavirus disease 2019 immediately increases burnout symptoms in ICU professionals: a longitudinal cohort study. Crit Care Med. 2021;49(3):419–427.
- Amsalem D, Lazarov A, Markowitz JC, et al. Psychiatric symptoms and moral injury among US healthcare workers in the COVID-19 era. BMC Psychiatry. 2021;21(1):546.
- Lai J, Ma S, Wang Y, et al. Factors associated with mental health outcomes among health care workers exposed to coronavirus disease 2019. JAMA Netw Open. 2020;3(3):e203976.
- Pfefferbaum B, North CS. Mental health and the Covid-19 pandemic. N Engl J Med. 2020;383(6):510–512.
- Schwartz RM, McCann Pineo M, Bellehsen M, et al. The impact of physicians’ COVID-19 pandemic occupational experiences on mental health. J Occup Environ Med. 2022;64(2):151–157.
- Marvaldi M, Mallet J, Dubertret C, et al. Anxiety, depression, trauma-related, and sleep disorders among healthcare workers during the COVID-19 pandemic: a systematic review and meta-analysis. Neurosci Biobehav Rev. 2021;126:252–264.
- Luo M, Guo L, Yu M, et al. The psychological and mental impact of coronavirus disease 2019 (COVID-19) on medical staff and general public—a systematic review and meta-analysis. Psychiatry Res. 2020;291:113190.
- Rossi R, Socci V, Jannini TB, et al. Mental health outcomes among Italian health care workers during the COVID-19 pandemic. JAMA Netw Open. 2021;4(11):e2136143.
- Hlubocky FJ, Back AL, Shanafelt TD, et al. Occupational and personal consequences of the COVID-19 pandemic on US oncologist burnout and well-being: a study from the ASCO clinician well-being task force. JCO Oncol Pract. 2021;17(7):e427–e438.
- Maftei A, Holman AC. The prevalence of exposure to potentially morally injurious events among physicians during the COVID-19 pandemic. Eur J Psychotraumatol. 2021;12(1):1898791.
- Frank E, Zhao Z, Fang Y, et al. Experiences of work-family conflict and mental health symptoms by gender among physician parents during the COVID-19 pandemic. JAMA Netw Open. 2021;4(11):e2134315.
- Cohn SK. Pandemics: waves of disease, waves of hate from the plague of Athens to AIDS. Hist J. 2012;85(230):535–555.
- Artiga S, Rae M, Pham O, et al. COVID-19 risks and impacts among health care workers by race/ethnicity. Kaiser Family Foundation. 11 Nov 2020. https://www.kff.org/report-section/covid-19-risks-and-impacts-among-health-care-workers-by-race-ethnicity-methods/. Accessed 10 Feb 2022.
- Wu JH. Asian healthcare workers in the COVID-19 pandemic: a long road to recovery. Nat Med. 2021;27(7):1135.
- Yi S. I’m an Asian American doctor on the front lines of two wars: coronavirus and racism. The Lily. 21 Apr 2020. https://www.thelily.com/im-an-asian-american-doctor-on-the-front-lines-of-two-wars-coronavirus-and-racism/. Accessed 25 Jan 2022
- Chew QH, Chia FL, Ng WK, et al. Perceived stress, stigma, traumatic stress levels and coping responses amongst residents in training across multiple specialties during COVID-19 pandemic-a longitudinal study. Int J Environ Res Public Health. 2020;17(18):6572.
- Maunder RG, Lancee WJ, Balderson KE, et al. Long-term psychological and occupational effects of providing hospital healthcare during SARS outbreak. Emerg Infect Dis. 2006;12(12):1924–1932.
- Phua DH, Tang HK, Tham KY. Coping responses of emergency physicians and nurses to the 2003 severe acute respiratory syndrome outbreak. Acad Emerg Med. 2005;12(4):322–328.
- Chan AO, Huak CY. Psychological impact of the 2003 severe acute respiratory syndrome outbreak on health care workers in a medium size regional general hospital in Singapore. Occup Med (Lond). 2004;54(3):190–196.
- Shanafelt T, Ripp J, Trockel M. Understanding and addressing sources of anxiety among health care professionals during the COVID-19 pandemic. JAMA. 2020;323(21):2133–2134.
- Song YK, Mantri S, Lawson JM, et al. Morally injurious experiences and emotions of health care professionals during the COVID-19 pandemic before vaccine availability. JAMA Netw Open. 2021;4(11):e2136150.
- Brower KJ, Brazeau CMLR, Kiely SC, et al. The evolving role of the chief wellness officer in the management of crises by health care systems: lessons from the COVID-19 pandemic. NEJM Catal Innov Care Deliv. 2021;10.
- Magnavita N, Soave PM, Antonelli M. A one-year prospective study of work-related mental health in the intensivists of a COVID-19 hub hospital. Int J Environ Res Public Health. 2021;18(18):9888.
- Ford JD, Carter AS, Grasso DJ, Briggs-Gowan MJ. The epidemic-pandemic impacts inventory (EPII) supplemental healthcare module-brief version (EPIISHMb). University of Connecticut School of Medicine. 2020.
- Schwartz RM. Understanding and addressing the mental health needs of healthcare workers and school staff during the COVID-19 pandemic. Poster presented at: The 37th annual meeting of International Society for Traumatic Stress Studies (ISTSS); Nov 2021; virtual meeting.
- National Academies of Sciences, Engineering, and Medicine; National Academy of Medicine; Committee on Systems Approaches to Improve Patient Care by Supporting Clinician Well-Being. Taking Action Against Clinician Burnout: A Systems Approach to Professional Well-Being. National Academies Press (US); 2019.
Category: Past Articles, Raising the Standard




