Lack of Weight Loss Differences with Differing Bougie Sizes in SADI-S: A Prospectively Collected, Retrospectively Analyzed, Matched Cohort Analysis

by Austin Cottam, MD; Daniel Cottam, MD; Olivia Johnson; Samuel Cottam, BS; Amit Surve, MD; Christina Richards, MD; Walter Medlin, MD, FACS
All authors are with Bariatric Medicine Institute in Salt Lake City, Utah.
Funding: No funding was provided for this article.
Disclosures: Dr. Daniel Cottam does consulting work for Medtronic outside of this work. All other authors report no conflicts of interest relevant to the contents of this article.
Bariatric Times. 2023;20(3–4):12–15.
Abstract
Background: There are currently no manuscripts comparing the efficacy of different bougie sizes in single anastomosis duodenoileal bypass with sleeve gastrectomy (SADI-S). This manuscript seeks to account for differences in bougie size (40 vs 48 French) in terms of weight loss and surgical outcomes.
Methods: Data from 960 patients who received SADI-S from four different surgeons were analyzed. Patients with 40 French bougie were separated and matched to those with 48 French bougie by age, sex, body mass index (BMI), and comorbidity status. Weight loss and complication data was collected up to two years postoperatively.
Results: Eighty-eight patients with 40 French bougie were compared to 88 patients with 48 French bougie size in a matched cohort design. Preoperatively, there was no significant difference between age, sex, BMI, or comorbidity status. At two years and 100 percent follow up, there was no significant difference in mid-term weight loss or complications.
Conclusion: Bougie size does not seem to impact the short-term or mid-term weight loss or complications associated with SADI-S.
Keywords: Bougie, weight loss, SADI-S, matched cohort analysis
When the single-anastomosis duodenoileal bypass with sleeve gastrectomy (SADI-S) was introduced in 2007 by Sánchez- Pernaute et al,1 the procedure was done with a bougie size of 54 French and a 200cm common channel. In response to issues with diarrhea and malnutrition, the common channel was lengthened to 250cm, while no change was made in the sleeve gastrectomy size. This change did indeed lower the complication rate but also resulted in less weight loss.2 The relative contribution of the sleeve gastrectomy (SG) to the weight loss that patients experienced after SADI-S was unresolved since this variable was held constant between the 200cm and 250cm common channel.2
Optimal bougie size has been a long-debated topic in the SG literature. As of yet, there have been no clear decisions made on the uniform bougie size needed for the SG. In the literature, many articles point to bougie size making a difference on weight loss, complications, and hospital stay, but just as many point to bougie size making no difference at all.
This topic of bougie contribution to short- and mid-term weight loss outcomes of SADI-S as of yet remains unexplored in the surgical literature. We present the first manuscript to compare bougie sizes in SADI-S by looking at the difference in weight loss and complications between 40 and 48 French through the use of a matched cohort design.
Methods
This study has been approved by the Quorum institutional review board (IRB) (QR# 31,353). Data was pulled from 960 patients from September 2011 to April 2021 who had been operated on by four surgeons at a single institution. In November 2017, one surgeon started performing this procedure with a 48 French bougie size, while the rest of the practice continued to use a 40 French bougie. During this time period, 88 patients underwent a SADI-S with a 48 French bougie.
This study uses a retrospective matched cohort design. All 88 of the 48 French bougie patients were matched to similar patients in the remaining 872 patient cohort who had received a 40 French bougie. These patients were matched on sex, body mass index (BMI; within 1 point), age (within 10 years), and similar comorbidity profile. Measured comorbidity status was based on diagnosed conditions of hypertension (HTN), gastroesophageal reflux disease (GERD), hyperlipidemia (HLD), obstructive sleep apnea (OSA), and Type 2 diabetes mellitus (T2DM).
Postoperative data measured was BMI and percentage excess BMI loss (EBMI). Excess BMI is defined as anything greater than a BMI of 25kg/m2. Data was collected for weight loss at three-, six-, 12-, 18-, and 24-months postoperatively. Short-term (<30 days) and long-term complication data was gathered and analyzed.
Continuous variables are presented as means with standard deviations, and categorical variables are presented using frequencies. Demographics were compared using paired t-tests and Chi-squared analysis. Weight loss outcomes and complication rates were compared using t-tests and Chi-squared analysis. A p-value of less than 0.05 was considered significant. All statistical analysis was done using R statistical software.
Surgical technique. Our technique for performing the SADI-S has been described previously.3 However, due to this work focusing on bougie size, all sleeves were performed by stapling alongside a 40 or 48 French bougie placed on the lesser curvature. No patient in the study had their staple line oversewn or reinforced. The staple line in all patients was started approximately 5cm from the pylorus and ended at the angle of His. Each patient had a visual inspection of the hiatus to evaluate for hiatal hernia, with simultaneous repair if a defect was found. The only difference in technique is that one group’s SG was constructed using a 48 French bougie, and the other was constructed using a 40 French bougie. All stapling techniques and other operative techniques were equivalent between groups.
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standard. For this type of study formal consent is not required. Informed consent was obtained from all individual participants included in the study.
Results
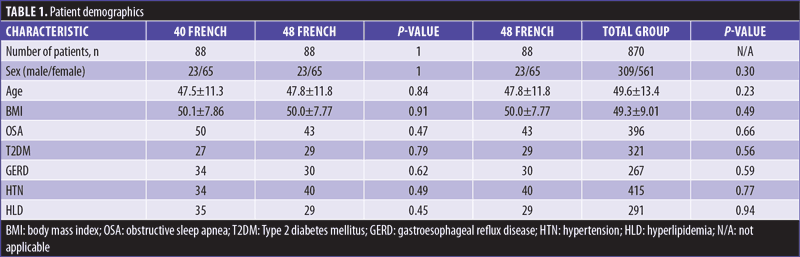
Overall, 176 patients were identified for our analysis. Demographics are found in Table 1. There was no significant difference in either group in sex, age, and BMI. There was no significant difference found in proportions of OSA, GERD, HTN, T2DM, and HLD. A comparison was made between the 88 matched 48 French patients against the general SADI-S with 40 French bougie. The results of this are also found in Table 1. There was no significant difference in any measured category found.
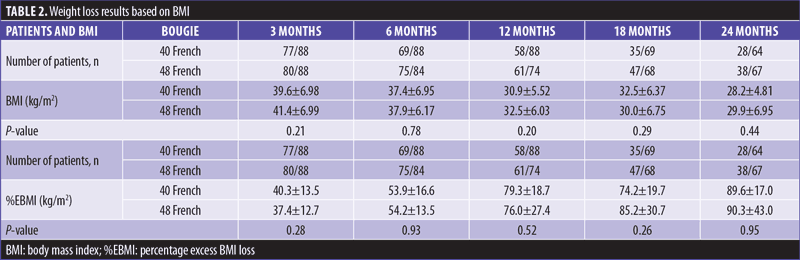
Weight loss results in terms of BMI are found in Table 2. Weight loss results from EBMI lost are also found in Table 2. There were no significant differences found between any time period studied.
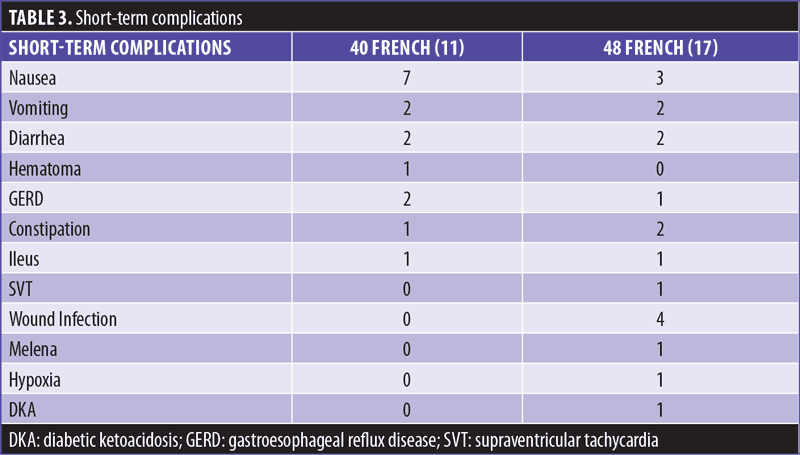
Short-term complications are shown in Table 3. There was no statistical difference in the number of patients with short-term complications between the two groups (p=0.26). In the 48 French group, there was one patient who had ileus postoperatively that could not be explained and required an esophagogastroduodenoscopy (EGD) and colonoscopy. No issue was found on exam. The patient eventually resolved and was discharged home. There was another patient who had a duodenal hematoma that required reoperation the same day. Besides these two patients, all other complications were handled through outpatient medication without admission.
In the 40 French group, there was one patient who required an EGD and colonoscopy due to hematochezia. No sources were found for the bleeding, and the bleeding eventually subsided without any significant drops in hemoglobin. No patients required operative management for their complications, and any other complications were resolved with medication without admission.
Mid-term complications are found in Table 4. There was no significant difference in complication rates between the two bougie sizes (p=0.56). In the 48 French bougie group, there was one patient with aggressive vomiting and dysphagia that required an upper gastrointestinal series and EGD that showed no stricture, leak, or narrowing. Another patient had new onset GERD after the surgery and was shown to have a hiatal hernia that required repair with resolution of symptoms. One patient in this group had a pulmonary embolism that led to their death, despite use of anti-Xa inhibitors for 30 days postsurgery.
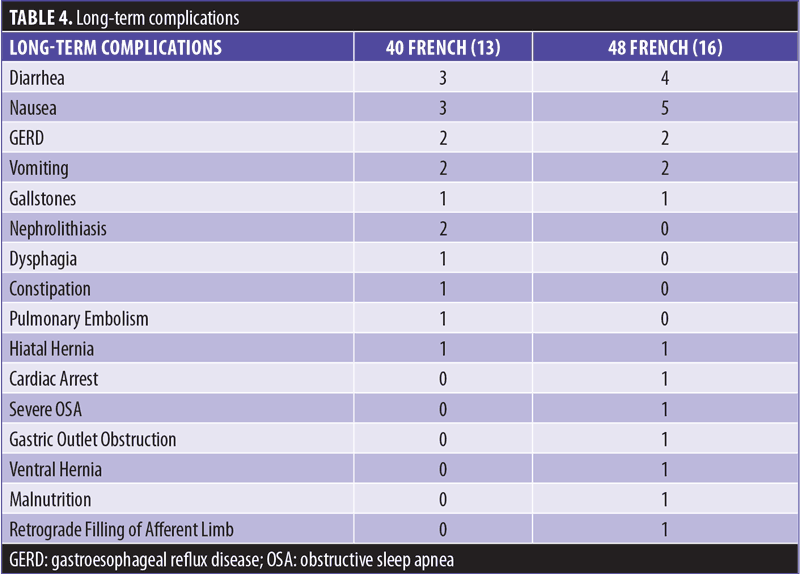
In the 40 French group, there was one patient who had a ventral hernia that required reoperation. There was another patient, who due to excessive diarrhea, was found to have retrograde filling of the afferent limb. She was reoperated on with the afferent limb being tacked on to the sleeve and the common channel lengthened from 300cm to 450cm. There was another patient who suffered from a gastric outlet obstruction requiring reoperation. There were two deaths in the 40 French group, one from cardiac arrest due to an unknown etiology more than six months after surgery and another death due to severe untreated OSA that was discovered at the time of surgery. The patient with severe OSA was unwilling to engage in any known treatments for OSA and left against medical advice, did not go to an emergency department with chest pain, and eventually expired at home.
Discussion
This is the first study of its kind to compare weight loss and complication outcomes between different bougie sizes in any duodenal switch (DS) or SADI-S. Bougie size has never been standardized due to its indeterminate effects on weight loss and complication profile. This choice has been almost entirely determined by individual surgeon preference and this is also true in Europe, Asia, and North America.3–5
In the literature available on sleeves and the effect of bougie size, there is not much consensus. In regards to weight loss, there are many manuscripts that have tried to determine the effect that bougie size has on weight loss. They all have used a wide variety of bougie sizes from 32 to 60 French. In three papers, there was found to be some difference in weight loss, favoring a smaller bougie size having greater weight loss.6–8 In five different manuscripts, no impact of different bougie sizes on weight loss was found.9–13
In terms of complication profiles with different bougie sizes, it has been hypothesized that a smaller bougie could have a greater chance of having a stricture or higher leak rate. In our own data, we did not see any statistically significant differences in complications in the short- or long-term. Since there are not many studies looking into the differences between bougie sizes in SADI-S, we should look to the SG literature for guidance.
In a meta-analysis from Yuval et al,14 they look at 4,999 different patients who underwent SG. They found a leak rate of 0.92 percent in a 40 French and a leak rate of 2.67 percent in anything smaller than 40 French. This difference was significant.14 Wang et al15 showed, through a meta-analysis of 6,608 patients, no significant difference in postoperative leak, overall complication, and GERD rates. Other, smaller manuscripts have shown inconclusive evidence on the effects of bougie size on complication rates.9,16–18 Our results fit into this narrative that there is no conclusive evidence to point, one way or another, to bougie size impacting complication rates.
Weight loss and complication results of our cohorts were favorably compared to other long-term studies presented in the literature. Our weight loss is statistically similar at 12 and 24 months to multiple studies.19–21 Additionally, our major complication rate was within the same margin as these other manuscripts.
Limitations. This study had several limitations. The first one was the small group size presented here. Similar group size has previously been used to study the effects of different bougie size in SG patients. Additionally, while each cohort in this study is small, our matched comparison allowed us to have better power than an unmatched design with a similar sample size. We matched each 48 French patient on a very tight basis to our other available patients with a 40 French size. Basing our matching on BMI, age, sex, and comorbidity status allowed us to cancel out any effects of our groups being different on a demographic basis that could have an effect on our results and analysis. It is well known that BMI, age, sex, and some comorbidities have been shown to impact weight loss. Our matching helped to get rid of this. Due to this study design, while it is possible that the smaller bougie size does still correlate to a difference in weight loss, this difference is likely to be small and might not be clinically relevant. Additionally, when doing small matched cohorts, these studies are never sufficiently powered to detect rare complications, and the complication data supplied here is only for the interest of the reader and is not statistically significant.
The second limitation of this study is the retrospective design. This design has some inherent flaws, but patient care was blinded, and none of our care staff knew which patients had smaller bougies and which ones did not. All of the follow-up care was the same, regardless of bougie size.
The third limitation is low follow-up in the 48 French group at 24 months. We attempted to reach out to all patients involved in this study to try to bring up this number, but many did not respond or no longer responded. While selection bias might be a factor in our results, this is unlikely to have made a large difference. The first reason is due to the research on patients who are lost to follow-up compared to consistently followed-up patients. In Hunter Mehaffrey et al,22 among patients who were lost to follow-up for 10 years, there was no difference in outcomes in terms of weight, comorbidity reduction, or complication profile, compared to those who consistently followed up.22 The second reason why our results would likely hold with higher follow-up is the very similar weight loss trajectories during the first six months, as they are almost identical, and follow-up is almost 80 percent. It has been previously shown in other bariatric procedures that the most predictive variable of future weight loss is short-term weight loss after surgery.23–25 As such, weight loss between the two groups would likely have been very similar at two years, since it was almost identical at six months.
The fourth limitation in this study is the small difference in bougie size. Especially with our small sample size, if the effect of bougie size was small, it would be hard to find. Future studies should examine the effects of larger differences in bougie size. However, this is strong evidence that relatively small changes in bougie size are unlikely to change outcomes in a single practice and can be left to surgeon preference.
Conclusion
Small differences in bougie size do not affect weight loss or complications in SADI-S patients. Further research should look into long-term effects of bougie size on complications, GERD resolution, and leak rates. Larger bougie sizes might need further study, since many SADI-S procedures are performed with bougie sizes 25 percent larger than the ones presented in this manuscript.
References
- Sánchez-Pernaute A, Rubio Herrera MA, Pérez-Aguirre E, et al. Proximal duodenal-ileal end-to-side bypass with sleeve gastrectomy: proposed technique. Obes Surg. 2007;17(12):1614–1618.
- Sánchez-Pernaute A, Rubio MÁ, Pérez Aguirre E, et al. Single-anastomosis duodenoileal bypass with sleeve gastrectomy: metabolic improvement and weight loss in first 100 patients. Surg Obes Relat Dis. 2013;9(5):731–735.
- Cottam A, Cottam D, Roslin M, et al. A matched cohort analysis of sleeve gastrectomy with and without 300cm loop duodenal switch with 18-month follow-up. Obes Surg. 2016;26(10):2363–2369.
- Li C, Lin S, Liang H. Single-anastomosis duodenal switch: conceptual difference between East and West. Obes Surg. 2021;31(7):3296–3302.
- Mitzman B, Cottam D, Goriparthi R, et al. Stomach intestinal pylorus sparing (SIPS) surgery for morbid obesity: retrospective analyses of our preliminary experience. Obes Surg. 2016;26(9):2098–2104.
- Hady HR, Olszewska M, Czerniawski M, et al. Different surgical approaches in laparoscopic sleeve gastrectomy and their influence on metabolic syndrome: a retrospective study. Medicine (Baltimore). 2018;97(4):e9699.
- Hawasli A, Jacquish B, Almahmeed T, et al. Early effects of bougie size on sleeve gastrectomy outcome. Am J Surg. 2015;209(3):473–477.
- Garay M, Balagué C, Rodríguez-Otero C, et al. Influence of antrum size on gastric emptying and weight-loss outcomes after laparoscopic sleeve gastrectomy (preliminary analysis of a randomized trial). Surg Endosc. 2018;32(6):2739–2745.
- Spivak H, Rubin M, Sadot E, et al. Laparoscopic sleeve gastrectomy using 42-French versus 32-French bougie: the first-year outcome. Obes Surg. 2014;24(7):1090–1093.
- Weiner RA, Weiner S, Pomhoff I, et al. Laparoscopic sleeve gastrectomy—influence of sleeve size and resected gastric volume. Obes Surg. 2007;17(10):1297–305.
- Abd Ellatif ME, Abdallah E, Askar W, et al. Long term predictors of success after laparoscopic sleeve gastrectomy. Int J Surg. 2014;12(5):504–508.
- Sánchez-Santos R, Masdevall C, Baltasar A, et al. Short- and mid-term outcomes of sleeve gastrectomy for morbid obesity: the experience of the Spanish national registry. Obes Surg. 2009;19(9):1203–1210.
- Parikh M, Gagner M, Heacock L, et al. Laparoscopic sleeve gastrectomy: does bougie size affect mean %EWL? Short-term outcomes. Surg Obes Relat Dis. 2008;4(4):528–533.
- Yuval JB, Mintz Y, Cohen MJ, et al. The effects of bougie caliber on leaks and excess weight loss following laparoscopic sleeve gastrectomy. Is there an ideal bougie size? Obes Surg. 2013;23(10):1685–1691.
- Wang Y, Yi XY, Gong LL, et al. The effectiveness and safety of laparoscopic sleeve gastrectomy with different sizes of bougie calibration: a systematic review and meta-analysis. Int J Surg. 2018;49:32–38.
- Atkins ER, Preen DB, Jarman C, et al. Improved obesity reduction and co-morbidity resolution in patients treated with 40-French bougie versus 50-French bougie four years after laparoscopic sleeve gastrectomy. Analysis of 294 patients. Obes Surg. 2012;22(1):97–104
- Aurora AR, Khaitan L, Saber AA. Sleeve gastrectomy and the risk of leak: a systematic analysis of 4,888 patients. Surg Endosc. 2012;26(6):1509–1515.
- Cal P, Deluca L, Jakob T, Fernández E. Laparoscopic sleeve gastrectomy with 27 versus 39 Fr bougie calibration: a randomized controlled trial. Surg Endosc. 2016;30(5):1812–1815.
- Sánchez-Pernaute A, Rubio MÁ, Cabrerizo L, et al. Single-anastomosis duodenoileal bypass with sleeve gastrectomy (SADI-S) for obese diabetic patients. Surg Obes Relat Dis. 2015;11(5):1092–1098.
- Zaveri H, Surve A, Cottam D, et al. Mid-term 4-year outcomes with single anastomosis duodenal-ileal bypass with sleeve gastrectomy surgery at a single US center. Obes Surg. 2018;28(10):3062–3072.
- Surve A, Cottam D, Medlin W, et al. Long-term outcomes of primary single-anastomosis duodeno-ileal bypass with sleeve gastrectomy (SADI-S). Surg Obes Relat Dis. 2020;16(11):1638–1646.
- Hunter Mehaffey J, Turrentine FE, Miller MS, er al. Roux-en-Y gastric bypass 10-year follow-up: the found population. Surg Obes Relat Dis. 2016;12(4):778–782.
- Mor A, Sharp L, Portenier D, et al. Weight loss at first postoperative visit predicts long-term outcome of Roux-en-Y gastric bypass using Duke weight loss surgery chart. Surg Obes Relat Dis. 2012;8(5):556–560.
- Cottam S, Cottam D, Cottam A, et al. The use of predictive markers for the development of a model to predict weight loss following vertical sleeve gastrectomy. Obes Surg. 2018;28(12):3769–3774.
- Cottam A, Billing J, Cottam D, et al. Long-term success and failure with SG is predictable by 3 months: a multivariate model using simple office markers. Surg Obes Relat Dis. 2017;13(8):1266–1270.
Category: Original Research, Past Articles




